
Our Insights.
Our Insights.
We are an insightful, well-connected bunch. So we have launched a video platform, Re_frame the Future, to show our connections and insights as we speak to change makers from across the industry and much further afield.
More Videos
Our deeper insights blogs and reports on the latest industry thinking.
Generative Engine Optimisation (GEO): Closing AI Gaps, Creating Market Edge
The way people find answers has changed. We used to chase blue links; now the answer shows up first, stitched together by AI. For life sciences, that shift isn’t cosmetic, it’s clinical. If generative engines can’t “see” your data, they won’t cite your brand or organisation. If they misread it, they’ll mislead your audience. Enter More…
The way people find answers has changed. We used to chase blue links; now the answer shows up first, stitched together by AI. For life sciences, that shift isn’t cosmetic, it’s clinical. If generative engines can’t “see” your data, they won’t cite your brand or organisation. If they misread it, they’ll mislead your audience. Enter Generative Engine Optimisation (GEO): the discipline of being accurately cited in AI answers, not just ranked in search.
Why GEO, why now?
SEO still matters. But AI assistants (ChatGPT, Perplexity, Gemini etc) increasingly aggregate and summarise, which means zero-click experiences are rising and traditional CTRs are falling. Visibility now hinges on whether engines understand your entity, trust your evidence, and can quote you clearly. That’s GEO: making your science legible to machines so humans get the right message.
When AI misleads
Spectrum Science recently shared a panel with NewAmsterdam Pharma, at Fierce Pharma Week, to unpack what GEO means for healthcare. NewAmsterdam shared that despite publishing updated Phase 3 clinical results and maintaining a clear SEO strategy, they found that AI tools continued to surface outdated Phase 2 data and references to historic failures in the same drug class. So whilst the web moved on, some AI answers… didn’t. As Bob Rambo, Executive Vice President of Marketing at NewAmsterdam put it: “AI gives you what seems like the truth, but it might not be accurate.” GEO exists to close that gap. You don’t want yesterday’s study writing tomorrow’s reputation.
GEO ≠ SEO (it’s SEO plus)
GEO builds on SEO, then pushes into three areas: citability, entity clarity, and distribution beyond your .com. Think: “help the robot help you.”
The GEO playbook
- Audit the answer engines
Use a third party tool to eliminate bias. Capture what AI says today about your brand, asset, MOA, class, and competitors. Log hallucinations, outdated claims, missing context. Prioritise high-risk fixes. - Fix the record
Update, redirect or retire legacy pages that anchor wrong answers. Add date stamps, study phase labels and “what changed” callouts. Publish post-read TL;DRs so models can lift accurate context in one grab. - Engineer citations (earned first)
LLMs over-index on high-authority sources. Land your proof points in credible third parties: peer-review commentary, top-tier health trades, guidelines, registries, respected KOL subsites. Treat digital PR as GEO fuel, not vanity. - Write for answers, not rankings
Structure pages the way engines compose: clear H2 questions, tight paragraph answers, bullet proof points, FAQs, and explicit definitions. Pair patient-plain explainers with HCP-precise detail. Add schema (Article, FAQ, Organization, Product/Drug where permissible) and robust author bios to strengthen E-E-A-T. - Optimise your entity
Use exact, unambiguous names for products, trials and endpoints. Align references across owned and earned channels. Where appropriate, ensure consistent facts on high-trust public sources (e.g., Wikipedia/Wikidata entries that meet notability and compliance standards). - Distribute beyond the website
AI engines learn from communities. Publish executive POVs on LinkedIn, time-stamped explainer videos on YouTube, and conference recaps in respected forums. Participate where policy allows (Reddit/Quora cautiously in pharma). Consistency builds brand-as-entity. - Mind the tech
Don’t accidentally block reputable AI crawlers if citations are a goal. Ensure Bing is set up (many assistants route through Bing). Maintain crawlability, clean internal linking and fast pages — not because speed “wins GEO,” but because broken sites rarely get cited. - Measure what matters
Evolve KPIs: track appearances in AI answers, referred sessions from assistants, assisted conversions, and brand-mention lift. Create a quarterly “prompt test” battery for priority queries. If you can’t measure it yet, at least monitor it consistently. - Rethink paid + organic
AI Overviews can displace ads and organic. Shift some budget to assets that win the excerpt (YouTube, high-authority placements, rich snippets). In creative, front-load the benefit and proof so your message survives summarisation. - Governance, always
Build GEO into MLR. Pre-approve canonical definitions, claims and data blocks you want quoted. Set policy on AI crawler access and attribution. Train teams to spot and report harmful AI answers quickly.
Conclusion: Don’t let the model write your story
The future of discovery is conversational, citation-driven and happening now. Brands that optimise for AI-driven answers will protect visibility, compress misunderstanding and win trust at the point of question. Aurora, as part of Spectrum Science, helps life sciences teams operationalise GEO, from audits and PR-powered citation plans, to answer-friendly content architecture and measurement.
AI isn’t the threat. Complacency is. Shape the narrative today, or the narrative will shape you tomorrow.
Turning Experience into Value: Europe’s Opportunity to Lead on Patient-Focused Medicines Development
The European Medicines Agency’s (EMA) Patient Experience Data (PED) reflection paper published last week signals a shift in expectations for how PED should shape medicines development and regulatory decisions in Europe. As the FDA re-orders its priorities under the oversight of Secretary of Health and Human Services, Robert F Kennedy Jr., this timely publication positions the EMA More…
The European Medicines Agency’s (EMA) Patient Experience Data (PED) reflection paper published last week signals a shift in expectations for how PED should shape medicines development and regulatory decisions in Europe. As the FDA re-orders its priorities under the oversight of Secretary of Health and Human Services, Robert F Kennedy Jr., this timely publication positions the EMA to potentially assume leadership in patient-focused medicines development.
EMA defines PED as data that directly reflects patient or caregiver experience—without input or interpretation by clinicians, third parties, or AI-based devices. PED encompasses health and functional status, symptoms, disease course, treatment preferences, quality of life, factors affecting adherence, outcomes, and side effects, as long as they are directly reported. PED is collected via quantitative (surveys, Patient Reported Outcomes), qualitative (interviews, focus groups), or mixed approaches, provided methodologies are robust and validated.
Historically, the FDA set the pace with practical, detailed guidance and templates, giving companies clarity on what’s required. Yet it’s still unclear how much PED influences regulatory decisions. The EMA’s reflection paper, now under public consultation, contends PED should be systematically considered throughout the entire medicines’ lifecycle. It goes further, emphasizing qualitative data and active patient group engagement to enhance relevance and inclusivity. If consistently applied, this approach could make PED central to regulatory assessment, health technology appraisal, and clinical practice.
The benefits of EMA taking on this leadership role are substantial for European research and healthcare: earlier and deeper patient involvement, improved trial and endpoint design, and sharper value propositions throughout development. In a climate where US-centric investment frequently dominates, a stronger European patient-focused approach could elevate the region as a clinical research destination—especially for studies requiring robust patient input and outcomes.
To truly lead, EMA must advance beyond encouragement. What’s needed now is clear, practical guidance. Just as importantly, stakeholders—including patients and advocacy groups—must see how PED gets assessed and weighed in regulatory and reimbursement decisions. This remains ambiguous on both sides of the Atlantic. Examples, feedback mechanisms, and honest dialogue about PED’s actual impact are vital for trust and progress.
If priorities of the FDA and EMA begin to diverge, global leadership and connectivity, combined with local understanding of how to navigate access hurdles in both regions will become more critical than ever.
At Aurora, a Spectrum Science company, our team of Patient Advocacy and Engagement experts sit alongside our clinical, commercial and communications colleagues, working harmoniously to ensure the critical information we gather from patients is actionable and pulled through at each stage of a product lifecycle. While many companies can gather patient data, few are as well positioned as Spectrum to be able to transform the insights gathered into lasting value for both patients and pharmaceutical companies. Contact us today to learn more.
Solving the patient engagement value equation
‘While there is plenty of exposure for patient engagement through the creation of worthy (and shiny) initiatives, the extent to which patient-focused medicines development is taking root is less clear’ Are we engaging with patients to impress our peers and stakeholders or to develop better medicines and support? Of course, both can be true at More…
‘While there is plenty of exposure for patient engagement through the creation of worthy (and shiny) initiatives, the extent to which patient-focused medicines development is taking root is less clear’
Are we engaging with patients to impress our peers and stakeholders or to develop better medicines and support?
Of course, both can be true at the same time. But while an improved reputation can be a by-product of patient engagement, it should not be the driving force behind it. Reputation enhancement is not the reason the US 21st Century Cures Act emphasised the need for patient engagement in medicines development or why the US Food & Drug Administration (FDA) and European Medicines Agency (EMA) actively drive a patient engagement agenda.
The legislation and regulatory support came into place because the benefits of patient engagement in medicines development have been well established: accelerating clinical trial recruitment; reducing protocol amendments; strengthening trial data and improving product viability.
In the current geopolitical climate and the uncertainties created for life sciences companies, it is more important than ever to look beyond the ‘patient- centric’ narrative or storytelling and instead demonstrate how patient engagement is driving improved outcomes for patients and the company.
A strategic and rigorous approach to patient engagement that demonstrates value creation for stakeholders and the life sciences company is vital if we are to address persistent scepticism, both internally among scientists and commercial teams and externally among stakeholders, including clinicians, regulators, payers, policymakers and even patients.
Such scepticism is often driven by concerns related to either:
- Tokenistic involvement to justify decisions
- The creation of research bureaucracy/ hoops to jump through
- Patient expertise to be involved in medicines development.
Yet, this scepticism is compounded when patient engagement is primarily leveraged as a driver of reputation. Pharma corporate collateral is dominated by phrases like ‘patient-centric approach’ but clear articulation of what this means or how it is measured isn’t usually provided. Furthermore, barely a month goes by without a major industry patient engagement event taking place – while best practice sharing is vital, the frequency of these events (often among industry representatives and patient advocates who are already familiar with the themes covered) raises some questions about the real motivation.
Only a handful of companies have published details of how they are systematically integrating patient engagement across the life cycle and how they are measuring its value. This is significant as currently no standardised tool exists to assess all aspects of patient engagement across the life cycle, leading to inconsistent benchmarking and lack of alignment on what success looks like. Patient-Focused Medicines Development (PFMD), a cross-industry collaborative, warrants mention here for contributing to a systematic approach (developing tools like the metrics selector and patient experience data navigator), but further validation is still required.
So, while there is plenty of exposure for patient engagement through the creation of worthy (and shiny) initiatives, the extent to which patient-focused medicines development is taking root and how its value is being measured is less clear.
At Aurora, a Spectrum Science company, we believe the key to creating value through patient engagement is found at the intersection of three core elements: deep scientific expertise and commercial acumen, along with advanced patient and stakeholder engagement capabilities.
Without understanding the scientific and commercial landscape in a deep way, patient engagement will be blunted in realising its potential as a strategic driver of innovation and growth.
Aurora’s patient engagement offering focuses on three vital points:
- Insights team: in-house patient research and analytics capability focused on generating rapid insights and evidence
- Strategic precision: breadth and depth of our capability maximises value of insights and unlocks new opportunities from preclinical to commercialisation
- Local to global: patient engagement expertise in 60+ markets globally, connected to networks of patient communities and proficient in local industry regulation.
Moving beyond patient engagement as a driver of reputation means building authentic, empathetic partnerships with patient communities, generating data and insights and applying it where it can make the greatest impact scientifically and commercially.
We need less talk about being patient- centric – and more thought, action and demonstration towards realising the impact for patients and companies.
Looking to solve your company’s patient engagement value equation? Get in touch.
Sustaining our commitment to a healthier planet
At Aurora, we believe that healthier people and a healthier planet go hand in hand. That belief drives not only the work we do with clients – helping to shape more sustainable healthcare – but also the actions we take to reduce our own environmental impact as a business. I’m proud to share that we More…
At Aurora, we believe that healthier people and a healthier planet go hand in hand. That belief drives not only the work we do with clients – helping to shape more sustainable healthcare – but also the actions we take to reduce our own environmental impact as a business.
I’m proud to share that we have now achieved Planet Mark Business Certification for the fifth consecutive year. This is an important milestone on our journey toward net zero, and one that reflects our sustained commitment to measuring, managing and meaningfully reducing our carbon footprint.
What we’ve achieved so far
Through our Planet Mark certification, we track emissions across a broad range of categories aligned with the internationally recognised GHG Protocol, ensuring that our progress is credible, transparent and independently verified.
Here are some highlights from our latest report:
🌍 We have reduced our market-based carbon footprint by 44% compared to the previous year
✈️ Business travel emissions have fallen by 46%, through a mix of changed behaviours and smarter travel choices
♻️Waste emissions are down by an impressive 72%, reflecting better management and improved recycling
📄 We are enhancing data quality and transparency year on year, building the foundations for future reductions
Our Scope 1 and 2 emissions remain at zero, reflecting our use of renewable energy and our London office’s energy-efficient profile. These include emissions we produce directly (like gas heating or company vehicles) and those from purchased electricity.
Currently, 100% of our measured emissions fall within Scope 3 — the indirect emissions that come from our wider value chain, such as business travel, procurement, and employee commuting. This is where we’re now focusing our efforts as we work toward a full organisational carbon footprint and long-term net zero goals.
What this means for us
Achieving our fifth year of Planet Mark certification is something the whole team at Aurora can be proud of. Sustainability is a shared responsibility and every step we take to reduce our impact helps build a healthier future for both people and planet.
Planet Mark certification is more than a badge; it’s a framework for continuous improvement and over the past five years, it has helped us to embed sustainability awareness and action into our day-to-day operations.
Where we go next
Our next steps will include:
📊 Expanding our Scope 3 reporting to capture all material emissions categories
🤝 Continuing to engage employees in our sustainability strategy, ensuring everyone has a role to play
⚙️ Exploring further operational improvements to support our long-term net zero ambitions
🌐 Enhancing collaboration with clients, partners, and suppliers to extend the impact of our sustainability efforts across the value chain
Why this matters
Climate change is a health issue. A more sustainable, resilient planet is key to improving human health and the health sector itself has an essential role to play in driving positive environmental change.
As a healthcare communications agency, we want to be part of that transformation, not only through the work we do with clients but also by taking responsibility for our own footprint and leading by example.
Sustainability is not a one-off project; it’s an ongoing journey. This fifth year of Planet Mark certification marks an important milestone, but we know there is much more to do. We remain committed to progressing further, faster and to contributing positively to both planetary and human health.
Between luck and leadership: Success because of, not despite, strategy.
While sounding like an obvious statement, strategic planning is pivotal in shaping long-term success. However, given the lack of rigour and time it is sometimes given, perhaps it is not so obvious. It can be argued many in our industry succeed despite their strategy, not because of it. A helpful way to think of strategy More…
While sounding like an obvious statement, strategic planning is pivotal in shaping long-term success. However, given the lack of rigour and time it is sometimes given, perhaps it is not so obvious. It can be argued many in our industry succeed despite their strategy, not because of it.
A helpful way to think of strategy is, as Lawrence Freedman defines it in his epic Strategy: A History, “getting more out of a situation than the starting balance of power would suggest.” Considering our world with this definition demonstrates how robust strategic planning can significantly influence market penetration, educational improvements, competitive differentiation, and patient outcomes.
Despite widespread acknowledgement of its importance, many companies still approach strategic planning inconsistently. One of the core challenges lies in our industry’s inherent complexity. From drug development cycles to stringent regulatory requirements, we operate in environments where uncertainty is the norm. Given this, we may say we recognise the crucial importance of competitive positioning, thorough market analysis, customer segmentation, and a clear value proposition. Yet, many teams fail to conduct the rigorous, data-driven evaluations necessary to adapt swiftly to changing market dynamics.
Flexibility is essential in environments we operate in, characterised by ongoing shifts in technology, professional stress, and patient needs. This means devising not only a formal plan but also implementing learning mechanisms to adapt quickly. Unfortunately, because strategic planning is often viewed as a one-time annual exercise, it does not continually evolve with real-world developments, leading to missed opportunities, underutilised resources, and suboptimal decision-making.
Done well, strategic planning can have a profound impact. Well-formulated strategies:
- optimise product portfolios,
- target the right patient populations, and
- align cross-functional teams around shared objectives.
They enable effective budget allocation, forge meaningful partnerships, and address specific unmet medical needs.
Ultimately, those who embrace a structured yet flexible approach to strategy creation and execution gain a sustainable long-term competitive advantage. Organisations recognising the value of ongoing, evidence-based strategy remain resilient, innovative, and adaptable in an ever-shifting landscape, succeeding because of strategy, not despite it.
If you want to strengthen your strategy and gain a competitive edge, get in touch with Chris Hall, our Strategy Director, to start the conversation.
Insights from the Pharma Social Media Conference 2025
On May 15th I attended the Pharma Social Media Conference in London. The sessions focused on how the pharmaceutical industry can build more effective and meaningful social media strategies, combining human creativity with new technology, while keeping trust and authenticity front and centre. A few key themes stood out throughout the day: the role of More…
On May 15th I attended the Pharma Social Media Conference in London. The sessions focused on how the pharmaceutical industry can build more effective and meaningful social media strategies, combining human creativity with new technology, while keeping trust and authenticity front and centre.
A few key themes stood out throughout the day: the role of AI, the importance of authenticity, and how to build trust in a space where audiences are increasingly turning for health information. We also heard practical examples of how companies are improving governance, collaborating across teams, and tailoring content to better meet the needs of both patients and healthcare professionals (HCPs).
Reaching patients and HCPs where they are
A point raised early in the day was how embedded social media now is in the healthcare journey for both patients and HCPs. 79% of users seek out social platforms to ask personal health questions. 77% start their treatment journey via a search engine. Platforms like Instagram, TikTok, and LinkedIn are already playing a role in how people learn about symptoms, treatment options, and how others are managing conditions.
50% of HCPs are now using social media for professional purposes, with LinkedIn ranked as the most trusted platform for engaging with scientific content. This is where we’re also seeing the rise of digital opinion leaders (DOLs); HCPs who bring clinical expertise into digital spaces through credible, and accessible content.
It’s important to develop content that aligns with the norms and expectations of each platform. Effective engagement is not just about having a presence, but on delivering content in a way that fits the context and audience
Misinformation travels faster than science
Several sessions focused on the link between content and trust. There’s a significant opportunity for pharma to build trust by sharing valuable, meaningful content, especially when we already have the science, data, and real-world stories to work with.
But facts alone don’t move people. Stories do. The strongest examples came from teams using content to connect emotionally with their audience whether by showing real patient experiences, using relatable storytelling.
Authentic content cuts through
Another strong theme was the need to prioritise authenticity. Content that feels overly polished or generic often fails to resonate, particularly on platforms like TikTok.
Influencer marketing was discussed as an effective way to build this kind of authentic connection. The emphasis wasn’t on high follower counts, but on relevance, credibility, and the ability to engage specific communities. Partnerships with patient advocates and digital opinion leaders can help bring pharma content to life in a more relatable way.
Employee advocacy was also highlighted as an underused but valuable approach. When employees talk about their work or share perspectives, it often feels more authentic and helps build credibility. But it has to be supported properly with clear guidance, guardrails, and a consistent tone.
AI brings possibility, but responsibility comes first
AI was mentioned throughout the day, with a focus on its practical uses across content creation, social listening, and internal processes. While it offers clear efficiencies and new capabilities, there was strong agreement that human input remains essential. Decisions around content strategy, tone, and audience engagement require contextual understanding and critical thinking. Especially in an environment where trust is critical and misinformation is common, the human role in shaping and validating content is key – as quoted from the panel Chair “One dodgy doctor can harm one patient at a time, one dodgy algorithm can harm thousands at a time.”
Compliance doesn’t have to be a barrier
Rather than viewing compliance as a barrier to innovation, a panel discussion highlighted the benefits of a more collaborative and solution-focused approach. The recommendation was to involve compliance teams early in the content development process to identify potential risks and opportunities together, rather than adapting content retrospectively.
Speakers encouraged a shift away from a purely risk-averse mindset, advocating for the use of the code as a framework to support and enable creativity. With clear governance in place, such as pre-approved messaging and agreed tone of voice, teams can operate with greater speed and confidence.
The overall message was to test ideas, challenge assumptions, and treat the code not as a constraint, but as a tool to create responsible, effective content.
Less content, more purpose
A final message of the day was around content strategy. Instead of pushing out high volumes of content, more teams are now focusing on making their content clearer, more relevant, and genuinely useful. Audiences are looking for content that helps them make informed decisions, reflects real experiences, and addresses the questions they actually have. As one speaker put it, it’s a choice to make quality content. Creating content that tells a clear, compelling story is key to capturing attention and driving behaviour change.
What next? Let’s talk about elevating your social strategy
Pharma’s social moment isn’t just coming, it’s already here. Delivering real impact in this space means balancing empathy with innovation, and creativity with governance. At Aurora, we help clients craft purposeful, creative content strategies that build trust, spark engagement, and make a difference.
If you’re looking to elevate your social media approach, from building trust with patients and HCPs to integrating AI responsibly and working confidently within compliance, we’d love to talk. Get in touch: hello@auroracomms.com
Navigating an increasingly complex oncology landscape with a view from the APEX
We have witnessed a radical transformation in cancer care in the last 20 years with the rise of immunotherapy, targeted therapies, precision medicine, alongside advancements in surgery, diagnostics and patient support. Cancer is a less prevalent cause of death today than it was at the turn of the Century. Despite great progress (Cancer Research UK More…
We have witnessed a radical transformation in cancer care in the last 20 years with the rise of immunotherapy, targeted therapies, precision medicine, alongside advancements in surgery, diagnostics and patient support.
Cancer is a less prevalent cause of death today than it was at the turn of the Century. Despite great progress (Cancer Research UK puts the fall in prevalence of death caused by cancer at 16% in that period), there is still major work to do to eradicate it as a major killer.
While innovation in oncology holds great promise, the challenges in bringing it to patients are becoming ever more complex:
- Limited and unequal access to diagnostic testing
- Difficulty generating evidence among smaller patient populations
- New patient populations emerging, including a rise in cancer incidence from those in under 50s of certain cancers
- Crowded industry pipelines with limited differentiation between products
- Shifting regulatory and payor landscapes
- Multiple competing priorities for limited health system budgets
These challenges are a shared problem for all parties: health systems trying to maximise population health from limited resources, clinicians seeking to prescribe the best therapies for their patients, and patients valuing improvements in survival and quality of life.
Collaboration is often talked about as a panacea that can help overcome many of these challenges but the reality for many stakeholders (already under pressure due to the demanding nature of their core responsibilities) is that they may struggle to find the time and or head space needed to engage meaningfully.
It is within this complex, noisy and busy environment that life science companies look to launch new innovation.
How Aurora can help
At Aurora, this is a world in which we are very familiar and one in which we are deeply experienced helping our clients to navigate to create genuine impact with product launches.
Our approach is always strategy-driven using our proprietary APEX model; we take an in-depth look at the landscape, understanding the barriers and motivators for engagement of all priority stakeholders and identify traction-winning territory for our clients versus their competitors.
Four reasons why Aurora is an essential strategic partner for industry working in oncology:
- Integrated offering: Our team includes experts across strategy, creative, communications, marketing and patient engagement who integrate to drive measurable progress for our clients.
- Proven track record: We understand the oncology landscape and work with our clients to generate strategic solutions thanks to our in-depth experience across multiple solid tumour types as well as haematological malignancies.
- Precision in client service: We pride ourselves on working as an extension of your team, operating with agility and a collaborative ethos to co-create solutions that drive lasting impact in oncology.
- Local insight drives Global impact: Oncology is a truly Global health priority, requiring joined up solutions. With offices in London, Washington D.C., New York and Chicago and a network of healthcare specialist agencies in 60+ markets, we create Global impact by connecting local expertise and insight.
We know what happens when product launch falls flat; stakeholder apathy, reputational stagnation and a commercialisation that is remembered for the wrong reasons or not at all.
Keen to learn more?
This is the first in a series of articles on oncology. The next will focus on our experience. If you would like to set up a call to learn more, please contact stephen.ofarrell@auroracomms.com.
Putting hearts at the heart of healthcare strategy
Cardiovascular disease (CVD) remains the leading cause of death globally, claiming 20.5 million lives in 2021. In the UK, it accounts for a quarter of all deaths and severely strains healthcare systems. Progress in tackling CVD is being made thanks to better screening, public health initiatives, new treatment innovations and digital health solutions. However, lifestyle-driven More…
Cardiovascular disease (CVD) remains the leading cause of death globally, claiming 20.5 million lives in 2021. In the UK, it accounts for a quarter of all deaths and severely strains healthcare systems.
Progress in tackling CVD is being made thanks to better screening, public health initiatives, new treatment innovations and digital health solutions. However, lifestyle-driven prevalence and disparities in care persist and the global burden of CVD is projected to rise by 90% by 2050, underscoring the need for deeper investment to drive transformative innovation.
Navigating Challenges and Opportunities
Our clients are tasked with bringing novel therapies to market within this complex environment. In addition to external factors, biotech commercial and medical teams often operate with limited internal resources, balancing competing priorities.
At Aurora, we specialise in global product commercialisation. We focus on seamless integration with our clients to provide integrated strategic, medical, patient-focused and commercial expertise, underpinned by proven methodologies and case studies.
Four reasons why Aurora is an essential strategic partner for industry working in CVD:
- Integrated offering: Our team includes experts across strategy, creative, communications, marketing and patient engagement who integrate to drive measurable progress for our clients.
- Proven track record: We understand the CVD landscape and work with our clients to generate strategic solutions thanks to our in-depth experience with chronic heart failure and lipid disorders.
- Precision in client service: We pride ourselves in working as an extension of your team, operating with agility and a collaborative ethos to co-create solutions that drive lasting impact in CVD.
- Local insight drives Global impact: CVD is a truly Global health priority, requiring joined up solutions. With offices in London, Washington D.C., New York and Chicago and a network of healthcare specialist agencies in 60+ markets, we create Global impact by connecting local expertise and insight.
A Call to Action
The future of CVD care is full of potential, but real progress depends on collaboration, innovation, and clear, impactful communication. As personalised medicine, AI-driven diagnostics, and regenerative therapies redefine the landscape, our promise is to be your dedicated strategic partner, helping to shape the landscape for innovation to succeed by fostering stakeholder understanding and action.
Because matters of the heart are at the heart of what matters in healthcare.
Keen to learn more?
This is the first in a series of articles on CVD. The next will focus on our experience in chronic heart failure and lipid disorder. If you would like to set up a call to learn more, please contact me at stephen.ofarrell@auroracomms.com.
Creative strategy in medical communications
The medical communications (med comms) industry is critical in bridging the gap between new medical innovations, healthcare professionals (HCPs) and patients. Without it, HCPs would have less access to education regarding scientific advances that could transform patient care. However, we are a long way from an optimal approach. An analysis by Veeva found that 20% More…
The medical communications (med comms) industry is critical in bridging the gap between new medical innovations, healthcare professionals (HCPs) and patients. Without it, HCPs would have less access to education regarding scientific advances that could transform patient care.
However, we are a long way from an optimal approach. An analysis by Veeva found that 20% more content was created throughout 2022 vs 2021, but 77% was rarely or never used in the field.
Furthermore, medical teams have often been siloed within the pharmaceutical industry, garnering a reputation that portrays them as highly scientific, reactive and lacking in creativity.
Times have changed and med comms doesn’t have to mean dry, clinical exchange – it should be slick and creative. Businesses increasingly regard medical affairs as a key strategic pillar. Industry trends show increasing collaboration between commercial and medical to deliver creative communication strategies. But why?
Rapidly evolving treatment landscapes and increasingly complex healthcare systems have led to an unprecedented transformation in educational needs.
The advent of omnichannel capabilities has shifted emphasis to integrated and personalised physical, digital and immersive learning. With this comes a significant need to blend strategy and creativity to ensure content remains engaging while not creating fractured messaging or information.
Innovation and adaptability
Learning preferences among HCPs have changed over recent years, with interactive, digital and bite-sized education among the most favoured approaches.
The med comms industry is adapting to these changes by providing strategic solutions that fit seamlessly into demanding schedules and reinforce learning through creative, immersive channels. For example, Medscape provides HCPs with one of the largest online medical learning platforms featuring bite-sized modules personalised to user speciality and on-the-go accessibility. From a practical standpoint, the strategic blend of science and technology has provided HCPs with simulation training designed to replicate real-world clinical scenarios. This form of training is recommended in current clinical guidelines, including The European Guidelines for the Management of Major Bleeding.
Nonetheless, creative implementation of a strategy is not limited to big ideas and novel technology, but rather to finding original ways to address audience demands. While creativity often becomes a synonym for technology, the frequently lost definition of creativity is the ability to produce or use original and unusual ideas. In the rare disease field, where awareness is limited, conventional means of scientific exchange may be more appropriate for forging the foundations of optimal patient care. Although such approaches may appear less ‘creative’ at face value, deviating from the modern-day norm of digital solutions creates an original perspective on medical education. As originality forms the essence of creativity, we must understand the audience’s needs to demonstrate the broad spectrum of creativity.
Engaging diverse audiences in complex concepts
Intricacies around disease pathophysiology, drug mechanisms and clinical trial design/ analysis form the backbone of medical affairs. As such, the med comms industry has been associated with dense, jargon-heavy content that is difficult to understand and does not engage audiences.
However, this stereotype is not genuinely reflective. The art of effective med comms is the ability to distil complex concepts into digestible content that drives behaviour change. Creative execution of strategy ensures the right messages resonate with the right audience.
Strategic messaging and positioning must be coupled with creative delivery to maximise knowledge retention.
Communication, through innovative storytelling and data visualisation, is widely believed to support greater engagement with audiences than lengthy materials littered with complex datasets. This applies to patients and HCPs alike. The narrative often differs in presentation and focus across these groups; however, data visualisation has proved powerful enough to engage at all levels simultaneously and globally. A good example is the ‘Flatten the Curve’ infographic used during the COVID-19 pandemic to translate extensive epidemiology and healthcare resource data into a simple visual that ultimately drove dramatic changes in public behaviour and healthcare policies.
Conclusion
Creative medical communications are not only critical for maximising knowledge retention, but are actively sought after across stakeholder groups. However, creative solutions can only reach and mobilise desired audiences with careful strategic foresight and positioning. Strategy, scientific integrity and creativity must form the foundations of med comms to meet the evolving demands of new audience generations, promote positive behaviour change and improve clinical care.
Georgia Hartnell is Scientific Lead at Aurora Healthcare Communications
Excellence in Customer Engagement: Takeaways from the Reuters Pharma Customer Engagement Europe 2024 Conference
The Reuters Conference offered a fresh, much-needed lens on how the pharmaceutical industry should engage with healthcare professionals (HCPs) and patients. In an industry that often feels rigid and slow to evolve, this event showcased that the industry is starting to forge real in roads into omnichannel, taking learnings from other sectors’ mistakes and errors, More…
The Reuters Conference offered a fresh, much-needed lens on how the pharmaceutical industry should engage with healthcare professionals (HCPs) and patients. In an industry that often feels rigid and slow to evolve, this event showcased that the industry is starting to forge real in roads into omnichannel, taking learnings from other sectors’ mistakes and errors, and helping us to adopt best practice. Don’t get me wrong, everyone was clear that no one is doing this perfectly, end-to-end, but there’s examples of real progress. From human-centric marketing to content automation, here’s my take on what’s driving meaningful engagement in pharma today.
Moving Beyond Customer-Centric to Human-Centric Marketing
One major takeaway: today’s marketing must go beyond customer-centric—it has to be human-centric. The conversation is no longer just about targeting customers with relevant information; it’s about genuinely understanding them. Marketing 3.0, as presented at the conference, puts empathy at the forefront. Brands that can demonstrate they “get it”, who can meet people where they are and speak to their values; are the ones who will build lasting relationships.
Consider the incredible cognitive overload HCPs face right now. They’re not just looking for more content; they want resources that simplify their lives, help them feel understood, and address real pain points in their daily work. As pharma shifts to human-centric marketing, there’s a powerful opportunity to bridge the gap by creating truly supportive, empathetic content that resonates.
Offline Interaction Is Becoming More Meaningful With Omnichannel
Everyone agreed that omnichannel engagement is a fantastic way to build credibility, authenticity and value for customers. But there was a real sense that in all of this, we can’t forget that offline or physical interactions are still the biggest value companies bring to customers. That’s how true personalisation and relevance can be achieved.
Omnichannel engagement strategies need to geared to supporting these offline interactions by providing data on who engaged with what, how and when, to ensure these interactions become even richer. Its critical these physical interactions are recorded and analysed within the broader data stack, as they come with unrivalled insights.
Omnichannel doesn’t just happen, it takes commitment, time and a long term view
Omnichannel isn’t as easy as flipping a switch and off you go. It’s about understanding where different audiences are and what they’re looking for, then meeting them there. Whether that’s a digital check-in, a face-to-face meeting, or an automated update. The magic of omnichannel lies in its flexibility. When done right, it’s an approach that respects how every customer might have unique communication preferences and adapts accordingly. But its not going to happen overnight. We need to ensure we’re continually building our understanding of our customers over a long period of time, to create a unique and personal experience for all of them. The benefit of our industry is we’re data rich and this is only going to increase. With that AI will take more of a prominent role in how we engage and personalise our content. And we saw that the conference, companies are already hiring data analysts and scientists to ensure data is clean, sorted and ready for use.
Data-Driven Personalisation: Meeting People Where They Are
If there’s one superpower that omnichannel engagement gives the pharma industry, it’s the ability to personalise at scale. Thanks to data analytics and AI, we can now understand not just what information someone needs but when they need it.
Data-driven personalisation isn’t just a trend, it’s essential for delivering information that is both relevant and impactful. And let’s be real: nobody wants to be bombarded with generic messages that don’t apply to them. When done well, personalisation brings value to every interaction, making each touchpoint feel intentional and valuable. Plus, the smarter we get with data, the more we can predict what our customers will need next, which is a massive advantage in building trust.
Breaking Down Silos for a Unified Experience
One challenge (or opportunity, depending on how you see it) is the need to get various departments aligned on omnichannel strategies. It’s not enough for sales, marketing, and data teams to work in isolation — breaking down these silos is critical to delivering cohesive experiences. When functions collaborate, they can combine insights and create a strategy that amplifies every
Final Thoughts
The insights from the Reuters Conference were clear: if the pharmaceutical industry wants to be truly effective, it’s time to lean into empathy, innovation, and smart omnichannel strategies. With data-driven personalisation, collaborative approaches, and a flexible blend of digital and in-person engagement, pharma companies have a powerful toolkit at their disposal. At the end of the day, it’s about creating real value, not just ticking engagement boxes. As the industry adapts, those who lead with authenticity and care will undoubtedly set a new standard for meaningful, lasting customer relationships.
But to be clear, no one is doing this perfectly, end-to-end. So, if you’re on the starting step of thinking through how you’re going to deliver seamless, consistent and authentic content to your customers, don’t be afraid to fail.
Please get in touch if you would like any advice or chat about anything further.
Scope Summit Europe: 5 reflections
Last week we attended Scope Summit Europe to exchange knowledge and experience about clinical trial recruitment and patient engagement. This conference is growing steadily in popularity year-on-year as clinical teams look to address the growing complexity of protocols and challenges associated with enrolment. Our 5 reflections: 1. Decentralised clinical trials are here to stay. Well, More…
Last week we attended Scope Summit Europe to exchange knowledge and experience about clinical trial recruitment and patient engagement. This conference is growing steadily in popularity year-on-year as clinical teams look to address the growing complexity of protocols and challenges associated with enrolment.
Our 5 reflections:
1. Decentralised clinical trials are here to stay. Well, elements anyway
In his presentation, The Inconvenient Truth of Decentralised Trials, Novartis’ Reamonn Madden spoke about how DCTs are well advanced through the Gartner hype cycle (from the peak of inflated expectations through the trough of disillusionment and now at the slope of enlightenment.) The upshot? Elements of DCT will be maintained for populations who need them but they are unlikely to become a universal solution for all trial participants.
2. Patient-focused protocol design is happening but the need for speed is slowing down broad adoption
Chiesi’s Marisa Minetti and Ylenia Paleari shared a great example of how patient insights helped to influence the design of a protocol to make their trial less burdensome for patients. While a shining example of the power of patient engagement in shaping clinical development, the reality for many clinical trials is that these critical steps continue to be deprioritised in favour of speed of set up. Meanwhile, clinical trial protocols grow in complexity and inclusion/exclusion criteria become more stringent to meet regulatory requirements.
3. Diversity, Equity but Exclusion continues for some
Great efforts are being made to make clinical trial populations more representative. For example, Bayer’s Binita Patel and Astra Zeneca’s Jodie Allen and Liz Bristow shared learnings from their companies’ respective diversity strategies related to race, gender and sexual orientation. However, as a research audit by Emily Botto and Maria Flores of Tuft’s University revealed, more needs to be done by industry as a whole to be more inclusive of socioeconomically disadvantaged populations in clinical research.
4. E-PROs, not just for research
A lively panel discussion on the challenges and potential of e-PROs concluded that we already have the technology to be using these digital tools in a real world setting, which could help to unlock the promise of personalised healthcare. Tech solutions like the smart toilet hold particular promise in collecting a wide array of data, according to Bernhard Glombitza of Bayer. However, it was cautioned by Jacqueline Bowman, Foundation for the Rights of Citizens of Obesity, that greater patient involvement is needed in the design of e-PROs to ensure we’re asking the right questions and assessing the right outcomes.
5. Clinical trial success hinges on connecting the dots across specialist capabilities
Our personal reflection from Scope Europe is that significant value remains unrealised in the pursuit of optimal clinical research. The opportunity lies in the Science of Enrolment; dissolving silos across clinical, medical and patient affairs to deliver strategic, integrated solutions that touch all priority stakeholders and leave a lasting impact well beyond the trial itself.
As a Spectrum Science company, we converge our capabilities in clinical trial recruitment, communications, medical communications and advertising to unlock value for our clients at every stage of the healthcare continuum. We are the strategic partner that accelerates progress of medical innovation through clinical development, regulatory approval, commercialization and international expansion.
The pharmaceutical industry is in a global innovation recession. This is how to get out of it: think ‘Glocal’
The world is in shock. Pandemic ‘recovery’; cost of living crisis; rising inflation and geopolitical instability at an all-time high for a generation. We’re in the middle of a polycrisis, and that’s not all. Around 1.5 billion people will be going to the polls this year, as significant elections are taking place in more than More…
The world is in shock.
Pandemic ‘recovery’; cost of living crisis; rising inflation and geopolitical instability at an all-time high for a generation. We’re in the middle of a polycrisis, and that’s not all.
Around 1.5 billion people will be going to the polls this year, as significant elections are taking place in more than 50 countries which between them hold almost half of the world’s population.
Uncertainty, then, is a constant we have come to live with. The result of this, is that we have come to crave something many people shy away from: change.
Global change coming to life science is good for all.
The life science industry, often proving to be resistant to most existential crises and pressure, has faced unprecedented low levels of investment, M&A activity and, as a result, lagging clinical pipelines. 2023 saw the lowest number of clinical trial starts since 2018.
If the world is in shock, the industry needs a shock of its own to ignite the change that innovation needs. This change is round the corner.
‘Pipeline in a product’ therapeutics, along with new and complex modalities, that will transform medicine, and, if given the right access environment, will also necessitate a reset, or change, in how we treat disease. Countries are rapidly standing up modern health systems that can accommodate these new innovations (let’s park capacity for a second, because that’s an altogether different challenge) and this rapid expansion requires genuine global expertise.
According to Deloitte, one of the main reasons why larger biopharma organisations miss their growth targets is because of an inadequate understanding of market dynamics and a complete misunderstanding of customer needs. A shameful finding given the hyperconnected world we live in. In today’s world, there really is no excuse, and change is not being embraced to stay in sync with the world today.
A true worldview and ‘global’ expertise then are paramount. But there really is no such thing as ‘global’ when it comes to life sciences. With every border comes a new culture to embrace, a new set of compliance considerations to consider and a new health system to navigate. The reality is that our work needs to resonate with countries and regions far more diverse than the term ‘Global’ allows.
For global strategy to be a success, you need to think ‘Glocally.’
Overcoming tunnel vision by thinking ‘Glocal’
How we tell stories about breakthrough science and the value this delivers to countries with unmet needs, demands a worldview on a range of issues to make sure medicine gets into the hands of those who need it.
Recent changes to EU regulations (for example, the Clinical Trial Regulation and new Medical Device/IVD Regulation) and other market uncertainties, such as cross-border collaborations and their potential impact on market access, are making it increasingly difficult for biopharma and biotech to forge ahead.
For programmes to resonate (and results to follow), multiculture, diversity and the need to consider all stakeholders in the care pathway are important, and that requires more than just a local presence, it necessitates a true understanding of local market dynamics. That means:
- Ensuring clinical trial recruitment materials are trans-created, so they not only resonate in-market, but also, they engage sites and recruit patients, and protocols co-designed with patient experience data.
- Commercial strategies are built with worldwide insight, supporting activities designed to drive uptake of medicines and new technologies through creative-led medical communications.
- Market access plans need to be shaped with payors years in advance of a commercial launch, and the right data generated through clinical development programs to gain reimbursement.
- Building global integrated teams that deliver across time zones to deliver at pace with cultural and compliance understanding built in.
As innovation lays a path for companies to expand internationally, we need to re-calibrate our understanding of the needs of nations and regions and people in a way that demands genuine expertise.
Our clients need partners who understand all these challenges, and in fact are purposefully designed to address and embrace them. So, that’s what we’ve built.
A Global vision with local precision
With decades of experience across every region of the globe, we’ve witnessed firsthand how the nuances of local geographies and cultures influence each phase of drug development and commercialisation. These insights have shaped our approach, leading us to create a platform of services that operate in harmony across the globe, delivering results that are truly greater than the sum of their parts.
By integrating solutions from clinical trial enrollment and medical communications to consulting and advertising, we’ve created an ability to take a wide-angle view, offering comprehensive, end-to-end support that spans the entire lifecycle—from early clinical milestones through to launch and global expansion.
This strategic offering is deeply ingrained in our heritage and our long-standing commitment to Global Health Marketing and Communications (GHMC)—the world’s largest network of independent healthcare agencies. Together, we’ve seen the difference a strategic and sensitive approach to multi-market programmes can make, as part of a deep understanding of healthcare across markets, cultures and codes.
As we seek to deliver change, we need to embrace it. And that’s what a truly ‘global’ partner like Aurora is designed to do. If you want to see what this difference looks like, get in touch.
My unforgettable experience at Aurora
I can still remember how nervous I felt on the first day standing outside their building, worrying about the tasks I was going to do or about the people I was going to meet. This immediately changed as I walked in. As soon as I stepped through the doors, my anxiety disappeared. I was greeted More…
I can still remember how nervous I felt on the first day standing outside their building, worrying about the tasks I was going to do or about the people I was going to meet. This immediately changed as I walked in.
As soon as I stepped through the doors, my anxiety disappeared. I was greeted with welcomes and warm smiles from the staff, who made me feel right at home. They took me on a tour of the building, and I was immediately captivated by the stunning views of London from the windows. The sight of The Shard, St Paul’s Cathedral, and the iconic London Eye spinning in the distance was simply amazing.
Once I settled in, I was assigned a project; to plan a presentation on the positives and negatives of AI in healthcare. This topic was fascinating. When researching artificial intelligence, I explored how it can revolutionize healthcare by improving diagnostics, personalising treatments and overall making doctors lives much easier. At the same time, I examined the ethical concerns, such as data privacy and job displacement.
Presenting my project to the team at Aurora was exhilarating and a lot of fun as I loved receiving so much support and positive feedback. I think the project was such a great task as it built my confidence when presenting which is such a major life skill to develop.
As well as this, I was also shown how to use websites like Canva to create professional logos.
But my time at Aurora wasn’t just about work. I spoke to many people, learning about what their job was within Aurora. I loved listening to each of their own back stories, their interests and how they became a part of Aurora. I enjoyed going out for lunch; some of the staff would take me to food stands and restaurants and I would get a great sense of the community of London.
Overall, I have loved every second. I am so grateful that I have had the opportunity to come to London and experience what it is like working at Aurora.
How AI is helping to improve patient care
There are now countless incredible examples of how artificial intelligence (AI) is transforming patient care to predict and detect disease and personalise medicine. Less frequently heralded is AI’s influence on soft factors that are just as critical in ensuring high quality patient care. At the heart of patient care lies the patient-doctor dynamic. It’s well More…
There are now countless incredible examples of how artificial intelligence (AI) is transforming patient care to predict and detect disease and personalise medicine. Less frequently heralded is AI’s influence on soft factors that are just as critical in ensuring high quality patient care.
At the heart of patient care lies the patient-doctor dynamic. It’s well documented that good communication between both is essential to enable good outcomes and avoid medical errors. Conversely, breakdown in communication can lead to harm and suboptimal treatment.
Increasing shared decision making and improving health literacy are key components of the solution, but neither are straightforward fixes.
Can AI help to bridge the gap in understanding between doctors and patients?
Two recent studies involving ChatGPT and Google DeepMind suggest it can.
Google DeepMind has developed a conversational medical AI system called AMIE (Articulate Medical Intelligence Explorer) to support conversations and aide diagnosis. AMIE uses “a novel self-play based simulated environment with automated feedback mechanisms for scaling learning across diverse disease conditions, specialties, and contexts”.
In a pilot study, investigators pitted AMIE against GPs to evaluate performance across several criteria including, history-taking, diagnostic accuracy, communication skills, and empathy. The results show AMIE outperformed the GPs almost all criteria, demonstrating superior diagnostic accuracy and conversational capabilities.
Similarly, in a separate study conducted with ChatGPT, 195 randomly drawn patient questions from an online forum were answered by both doctors and the AI. The AI responses were preferred to those of the doctors and rated AI significantly higher for both quality and empathy.
Neither of these studies is suggesting that doctors be replaced by AI in communicating with patients or that AI is a replacement for shared decision making or health literacy among patients. But when 70% of people turn to the internet as their first source of health information, it is crucial to understand how AI will influence how we educate ourselves about health conditions.
AI can potentially transform patient understanding of vital information, while freeing up doctors to invest greater energy in practicing medicine, but it is not a panacea. Relationships are built by people after all.
Make sure you don’t miss our latest insights and thinking by subscribing to our LinkedIn Newsletter here!
Aurora Healthcare Communications awarded PIF TICK accreditation to become a ‘trusted information creator’
Aurora Healthcare Communications, a Spectrum Science Company, has today been awarded the PIF TICK – the UK’s only assessed quality mark for print and online health and care information – by the non-profit Patient Information Forum (PIF). To become a ‘trusted information creator’, the agency underwent an assessment showing it met 10 key criteria* so More…
Aurora Healthcare Communications, a Spectrum Science Company, has today been awarded the PIF TICK – the UK’s only assessed quality mark for print and online health and care information – by the non-profit Patient Information Forum (PIF).
To become a ‘trusted information creator’, the agency underwent an assessment showing it met 10 key criteria* so patients and the public can be assured that the information they are reading, watching or listening to is evidence-based, understandable, jargon-free, up-to-date and produced to the best possible standard.
Dan Wills, PIF TICK manager at the Patient Information Forum, said, “We are thrilled to welcome Aurora to our ever-growing community of accredited PIF TICK members. Accurate, accessible, evidence-based information is key to increasing patient empowerment and improving health outcomes.”
Aurora is one of the first healthcare communications agencies in the UK to have been accredited with the PIF TICK, joining an impressive cohort of over 140 organisations including NHS trusts, patient advocacy groups, such as Cancer Research UK and MS Society, and pharmaceutical companies including Astellas and MSD UK, as well as four individual health content creators.
“The increase of false health information has eroded public trust, which is the bedrock of good relations and practices in healthcare. Health information needs to be authentic and trustworthy, with the source of the information clear.” said Stephen O’Farrell, Head of Patient Engagement at Aurora. “As proud health information creators and communicators, the PIF TICK quality mark represents an important standard for patients and the public to be assured that our health information is of high quality and reliable.”
The PIF launched the PIF TICK in May 2020. In July 2021, PIF launched the website www.piftick.org.uk to raise awareness of PIF TICK accredited members and help people find trusted health information. The site also includes guides on topics including spotting false health information and understanding evidence.
Sarah Contiero, Senior Account Director at Aurora, commented, “Our rigorous approach to creating health information has been recognised by the Patient Information Forum. For our clients, that means any health information we create on their behalf – that adheres to the 10 key criteria incorporated in our approach – can bear the PIF TICK emblem.”
Aurora was recently included in PRWeek’s UK Top 150 Consultancies 2024, climbing two places since 2023 as a result of its focus on combining ability and agility to deliver increased value for its clients.
— ENDS —
Notes to Editors:
For more information, please contact:
Nathan McGlone
E: nathan.mcglone@auroracomms.com
T: 07850 775 669
About Aurora Healthcare Communications
Aurora delivers impact for clients through our unique blend of strategy-first thinking and creative innovation. All of our communication work is grounded in science, human insight and optimised by data to resonate with the relevant target markets. Our approach connects our service offerings together to ensure that deep insights, brilliant creativity and intelligent metrics are part of every program. With Aurora’s ability and agility, audiences are engaged and objectives are exceeded, always underpinned by excellence in client services.
You can find more information about Aurora at https://www.auroracomms.com/.
About the Patient Information Forum

PIF is a charitable organisation for people working in health information. It represents more than 300 members, including NHS Trusts, charities, private companies, freelance writers and academics. It offers expert advice to promote the creation of trusted, clear, evidence-based health information. You can find more information about PIF and the PIF TICK at https://piftick.org.uk/.
*PIF TICK criteria for organisations
- Systems: Information is created using a consistent and documented process
- Training: Staff receive ongoing training and support
- Need: Resources meet a genuine need
- Evidence: Information is based on reliable, up-to-date evidence which is communicated clearly
- Involving users: Users are involved in the development of information
- Health inequalities: Information is written to meet health and digital literacy, language and accessibility needs of the target audience
- Content and design: Information is clearly communicated, easy to access and navigate
- Feedback: There is a clear process for users to provide feedback
- Disseminating: Information is promoted to maximise reach
- Impact: The impact of information is measured
April Insights & Innovations: Ethical Dilemmas in AI, Future of NHS Funding, and Genomic Surgery
At Aurora we are constantly staying abreast of the latest trends and insights in healthcare and pharmaceuticals and we want to share these with you. You’ll see below a few of the recent things we have read that gave us pause or made us look at things differently, especially in relation to things that the More…
At Aurora we are constantly staying abreast of the latest trends and insights in healthcare and pharmaceuticals and we want to share these with you. You’ll see below a few of the recent things we have read that gave us pause or made us look at things differently, especially in relation to things that the Aurora team is working on. If any of these topics resonate with you or if you have insights to contribute, please don’t hesitate to reach out at chris.hall@auroracomms.com. Please click on each title to view the whole article.
World Health Organization. Benefits and risks of using artificial intelligence for pharmaceutical development and delivery
The WHO has recently released a broad-ranging summary of the potential for AI in the pharma industry. The paper examines that AI already touches the entire product development and marketing spectrum. It also focuses on the potential for AI to widen existing inequity for neglected populations. It raises interesting ethical dilemmas we must address when using AI regarding the fine balance between efficiency, commercial success, and public health benefits. Regardless of where we fall in terms of this balance, it does show the wide-ranging need for collaboration across society to truly reap the benefits of AI in the creation and use of medicines. Inevitably, industry needs to sit at the centre of this collaboration. Mistakes will be made, bad actors will take advantage of the technology, but success can come about if there is a focus on true collaboration, and development of actual shared goals.
Appleby, J et al., BMJ 2024;384:e079341. The BMJ Commission on the Future of the NHS: NHS funding for a secure future
Of course, those of us in the UK are bombarded with the seemingly inevitable downfall of the NHS. This nice summary looks at how best to secure the future of the NHS amid the changing landscape of AI, advanced therapies, and demographic changes. The paper presents a sensible balance of continuing to fund through taxation with the need for an immediate cash injection, alongside creating an independent office to provide an unbiased look at the state of healthcare in the near and far term. Inevitably, given that it is about the future of the NHS, it has already attracted some debate and pushback. We can at least cross our fingers (in hope, more than expectation) that an open and focused debate may help push us towards a somewhat better future and a more stable health system in the UK.
The King’s Fund. Illustrating the relationship between poverty and NHS services
Another sad fact relating to the NHS (and all health systems) is the effect of poverty on people’s ability to live healthy lives. Poverty, health inequity and the associated issues are hugely complex. At Aurora, we have looked at how health inequality affects cancer care; you can see this in the Cancer Equals report we collaborated with BMS on. This report in the King’s Fund (funded by the Joseph Rowntree Foundation) discusses how poverty affects people’s ability to access healthcare more broadly and how the NHS, as an organisation, can help the drive to tackle poverty. When you look at some of the recommendations (helping people access health systems, using data to find people in poverty, poverty-proofing services), it is clear industry could (and should) play a key role in this. Given many of the people in poverty are more likely to be living with long-term conditions, for which industry has innovative solutions, it makes not only ethical sense to help them access healthcare but also business sense. While some good examples exist, there is a big need for more work here.
I Rahman and J Barwell. Coll. Surg. Engl. 106(4). Genomic medicine for the 21st century
On a more positive note, this editorial discusses how genomics can be more broadly applied to surgical practice outside rare diseases. Using genomics to inform preventative surgery nicely encapsulates the fusion between old and new medical approaches. There are clear infrastructure, time, and IT challenges to implementing this more widely, alongside true ethical concerns about what the health system can access regarding our lifestyle and socioeconomic status. This will inevitably open up a whole new frontier of patient engagement. The catalyst for this approach was the now-completed 100,000 Genomes Project. The results of this have given rise to many medical and diagnostic investigations for patients across rare and infectious diseases, cancer and even COVID-19. It is a shame successful approaches to innovative thinking such as this are not celebrated more broadly. I suspect most of the public may not even know about the project.
Make a positive change for health this Earth Day
Climate health and human health are inextricably linked so this Earth Day 2024 the team at Aurora has been reflecting on what more we can do to protect our planet and make it a healthier place to live, both through our own actions and how we advise our clients. Climate change is no longer a More…
Climate health and human health are inextricably linked so this Earth Day 2024 the team at Aurora has been reflecting on what more we can do to protect our planet and make it a healthier place to live, both through our own actions and how we advise our clients.
Climate change is no longer a distant threat reserved for scientific debates or future generations. Its effects are manifesting now, with profound implications for human health. The relationship between climate change and health is multifaceted and complex, affecting various aspects of physical and mental well-being.
The WHO says, “Climate change is impacting human lives and health in a variety of ways. It threatens the essential ingredients of good health – clean air, safe drinking water, nutritious food supply, and safe shelter – and has the potential to undermine decades of progress in global health.”
Just think about that for a second. The decades of progress made in health diagnosis, treatment and care, diminished by the way we live our lives and treat the planet. It’s one step forward and two steps back. No wonder it’s the decade of action!
The facts are frightening. A quarter of all deaths (an estimated 14 million) globally are linked to the environment and 99% of the world’s population lives in places where air pollution levels exceed WHO guideline limits.
The impact of climate change on public health
One of the most immediate consequences of climate change is extreme weather events such as floods, hurricanes, heatwaves, and wildfires, which are increasing in scale, intensity, and frequency. These events not only cause immediate injuries and fatalities but also disrupt healthcare systems and infrastructure, leading to long-term health consequences. Heatwaves, for instance, can exacerbate cardiovascular and respiratory conditions, particularly among vulnerable populations such as the elderly and those with pre-existing health issues.
Climate change also contributes to the spread of infectious diseases. Rising temperatures and changes in weather patterns create favourable conditions for mosquitoes and ticks. This has led to the spread of diseases like malaria, dengue fever, and Lyme disease into regions where they were previously uncommon. Additionally, extreme weather events can compromise sanitation systems, leading to waterborne illnesses such as cholera and typhoid.
What can we do?
This might all seem too big for us to do anything meaningful about, especially as a small to medium-sized enterprise (SME). But at Aurora we believe that we have a responsibility – morally and legally – to do what we can to minimise the harm we do to the planet and change our practices to contribute to the NetZero target by 2050. After all, we have always had the ambition to improve lives and prove it. We have the opportunity to do this through our client work too, ensuring social and environmental considerations are central to our campaigns, and being mindful of business travel.
Reducing emissions of greenhouse gases through better transport, food and energy use choices can result in huge gains for health, particularly through reduced air pollution.
So, in 2020 we started by measuring our carbon emissions, working with PlanetMark, an internationally recognised third-party sustainability certification organisation. Having achieved PlanetMark certification in 2021, we pledged to reduce our carbon footprint year-on-year, through energy efficiency measures, transitioning to renewable energy sources, and adopting sustainable practices throughout our operations. For example, when moving office, we were able to select a company that exclusively uses renewable power sources. Workspace also marks Earth Day through sustainable events to get everyone involved.
This year, we have committed to measuring Scope 3 emissions, which cover all indirect emissions throughout our entire value chain, including staff commuting and purchased goods and services.
Beyond measuring, we educate our team to think more sustainably in their day-to-day work, for instance, when and how to travel, how to reduce waste and printing, and we try to use local suppliers where possible. We have discovered it is possible to contribute to the NetZero target collectively and individually.
Through PlanetMark certification we also know that we currently positively affect seven of the 17 UN Sustainable Development Goals (SDGs), also known as the “Global Goals”. We contribute to climate action, sustainable cities and communities, and responsible consumption and production, among others. This is important to our business, our team, our clients, all living things, and the planet.
Climate change poses a significant threat to public health, with far-reaching consequences for individuals and communities around the world. Recognising the interconnectedness of climate and health is crucial in mobilising effective responses to mitigate these impacts and safeguarding the health and well-being of current and future generations. All businesses have a vital role to play in this effort, and by taking proactive steps to reduce our environmental impact and promote health equity, we can contribute to a more sustainable and resilient future for all.
If you would like to know more about our environmental efforts or would like to know how we are helping clients in this space, please get in touch.
Optimising health in an ageing population. Good for the person, good for the system
The Silver Tsunami: [1-5] One of the undeniable global achievements in the 20th Century was the rise in global life expectancy. For example, since the founding of the World Health Organization in 1948, life expectancy globally has increased from 46 to 73 years (often referred to as the silver (or grey) tsunami). While this is More…
The Silver Tsunami: [1-5]
One of the undeniable global achievements in the 20th Century was the rise in global life expectancy. For example, since the founding of the World Health Organization in 1948, life expectancy globally has increased from 46 to 73 years (often referred to as the silver (or grey) tsunami). While this is cause for celebration, it provides a significant challenge in ensuring people live longer in good health.
As we look to the coming decades, the increases in multimorbidity (the presence of two or more chronic conditions simultaneously in one individual) are stark. While multimorbidity is not a problem only for older adults, its prevalence is much higher in older age groups. For example, in Scotland, 65% of people aged 65–84 years and 82% of people aged at least 85 years were affected by multimorbidity in recent years. By 2050, it is thought that nearly 15 million Americans over 50 will suffer from multimorbidity.
It is tempting for society to see ageing, in and of itself, as a disease and those getting older as becoming disease-ridden. However, we must forcefully push back against this.
We know ageing is likely responsive to changes or adaptations at an individual level to improve functional health. Low-cost interventions such as resistance training can be powerful interventions. Resistance training in older adults not only combats the loss of muscle strength and mass but improves physical functioning, mobility, independence, chronic disease management, psychological well-being, quality of life, and healthy life expectancy.
As we age, some changes occur in all organs; most changes can be primarily managed effectively. And while changes such as these and, ultimately, death are inevitable, disabling chronic illnesses are not.
Managing multimorbidity: [6-11]
Given the scale of the problem, it is no surprise that international action is underway. In its first review of good practices across Europe in 2013, the EU’s Action Group on Prescription and Adherence to Medical Plans identified a significant issue with polypharmacy and poor medication adherence amongst patients with multimorbidity, highlighting the increased risk of adverse events and hospitalisation associated with inappropriate prescribing.
Recent research has demonstrated improvements in multimorbidity management through both a system-level and a patient-centred approach. From our perspective and where we can have the most influence, the patient-centred approach is the most interesting and can be thought of in the following way:
- Improving health and digital literacy
- Building the healthcare professional-patient relationship
- Promoting shared decision-making and setting realistic goals
- Supporting self-management (for example, through ‘wearables’ tracking and real-world evidence generation)
These components comprise patient activation, which describes an individual’s willingness and ability to take independent actions to manage their health and care.
Several unmet needs for patient-centred care have been raised, which, for brevity, can be broadly grouped into the following categories:
- Lack of a holistic approach by different healthcare professionals (insufficient attention to the patient’s state of functioning, their limitations in daily life, and their well-being)
- Lack of personal continuity of care
- Lack of patient-tailored explanations about diseases and treatments
- Lack of social and mental health support
Additionally, these unmet needs are likely to be greater in ethnic minority groups and those from lower socioeconomic backgrounds.
The role of industry: [1,12-17]
This is most important for those in industry with Global or International remits. Not only is multimorbidity very common in wealthier nations, but around 80% of the world’s older population will live in low and middle-income countries by 2050. This must be considered carefully, given the dramatic impacts this could have, such as 71% of people with dementia living in these countries. However, given rapid technological advances, ageing does not have to be associated with worrying statistics. Happy, healthy ageing, where people contribute positively to society in a range of ways, can be a reality for most people, and while technology will undoubtedly be at the heart of it, the basics must be tackled first.
Industry can improve this situation straightforwardly based on the current unmet needs for multimorbid, older patients. The following initiatives can be focused on quickly and need not be cost—or resource-intensive.
Working directly with older, multimorbid patients:
- As patient involvement has become more sophisticated and more impactful, there remains a dearth of experience with older people. This is likely because of the apparent complexity of involving older adults and the belief that they may not be able to contribute as much as younger people.
‘Joined-up’ education:
- Given the polypharmacy of multimorbid patients, a truly patient-centred approach to care is crucial. Cross-disease, above-brand disease awareness could help older patients with treatment adherence, coping skills and quality of life.
Integrated physical and mental health care:
- The effect on self-reported health of mental health symptoms caused by physical illness is an increasing public health problem. As medicine advances and life expectancy increases, there are growing expectations to live a healthy life even in old age. Industry can provide specific integrated physical and mental health management education to older patients, helping them optimise their care beyond treatment.
How we work with these people must be addressed in everything we do. Older, multimorbid populations are more likely to be isolated and lonely and, therefore, hardest to reach. Alongside industry, a multi-stakeholder approach is needed to fully engage with this audience (social care, NHS, charities, community groups, etc). Additionally, we must consider the process in which we engage. Adjusting for digital capabilities, mobility for meetings, accessibility of contracts and so on. We must ensure SOPs and compliance can flex to this.
Where do we go from here?
Fundamentally, greater political will and increased resources are necessary to create a world where all people live long and healthy lives. However, the question remains within industry: what can we do to ensure healthier ageing?
There are clear gaps for industry to lend its expertise to provide significant value to multimorbid patients. This will not only improve adherence and reduce adverse events but also improve multimorbid patient management, which could substantially ease the stress on health systems as the predicted numbers increase over the coming years.
We must work together, working directly with older people, their families, and communities. Additionally, a more joined-up approach to disease education across relevant therapy areas, such as cardiovascular or respiratory, focused on the impact of healthy ageing with multiple diseases, could greatly benefit multimorbid patients. As creators of innovation, the responsibility falls upon industry to partner up and rise to this occasion. The imperative is clear: we must be the architects of a new dawn where everyone, regardless of age or ailment, finds health and happiness in a world that nurtures their well-being.
At Aurora, over our 18 years, we have focused on working closely with distinct groups of people when creating patient and healthcare professional education. We have significant expertise and case studies in this area. Our team of experts in patient advocacy, behavioural science and communications recognise the importance of proactive chronic illness management for the benefit of the individual patient, healthcare system and society. We have launched our All for Activation behaviour change approach to create effective, measurable interventions that aim to positively impact all stakeholders to achieve success with patient activation strategies. Get in touch if you’d like to hear more.
References:
[1]. WHO. Progress report on the United Nations Decade of Healthy Ageing, 2021-2023. Accessed January 2024.
[2]. Banerjee S. Multimorbidity—older adults need health care that can count past one. The Lancet. 2015:14;385(9968):587-9.
[3]. Fulop T, et al., Are We Ill Because We Age? Front Physiol. 2019;18(10):1508.
[4]. Fragala, Maren S. et al., Resistance Training for Older Adults: Position Statement From the National Strength and Conditioning Association. Journal of Strength and Conditioning Research 2019;33(8):2019-2052.
[5]. Jaul E and Barron J. Age-Related Diseases and Clinical and Public Health Implications for the 85 Years Old and Over Population. Front Public Health. 2017;11(5):335.
[6]. European Commission. Replicating and tutoring integrated care for chronic diseases, including remote monitoring at regional level 2013; Brussels: European Commission. http://ec.europa.eu/research/innovation-union/pdf/active-healthy-ageing/gp_b3.pdf#view=fit&pagemode. Accessed January 2024.
[7]. Rohwer, A. et al., Models of integrated care for multi-morbidity assessed in systematic reviews: a scoping review. BMC Health Serv Res 2023;23:894.
[8]. Health Affairs. What the evidence shows about patient activation. Available at: https://www.healthaffairs.org/doi/10.1377/hlthaff.2012.1061. Accessed: January 2024.
[9]. Jingjie Wu, et al., Healthcare for Older Adults with Multimorbidity: A Scoping Review of Reviews, Clinical Interventions in Aging, 2023;18:1723-1735.
[10]. Wagner C, et al., How life course socioeconomic conditions shape multimorbidity in old age – a scoping review, European Journal of Public Health, 2022;32(3).
[11]. Rolewicz L, et al., Are the needs of people with multiple long-term conditions being met? Evidence from the 2018 General Practice Patient Survey. BMJ Open 2020;10:e041569.
[12]. Alzheimer’s Disease International. Policy Brief for Heads of Government. The Global Impact of Dementia 2013–2050. https://www.alzint.org/u/2020/08/GlobalImpactDementia2013.pdf. Accessed January 2024.
[13]. Belcher, V.N., et al., Views of older adults on patient participation in medication-related decision making. J Gen Intern Med 2006;21:298–303.
[14]. Martine T.E. et al., Patient engagement in research with older adults with cancer. Journal of Geriatric Oncology. 2017;8(6):391-396.
[15]. Davis, S.F., et al. Hearing the voices of older adult patients: processes and findings to inform health services research. Res Involv Engagem 2019;5:11.
[16]. Jacobs, R and M. Kane. 9th annual International Conference of Education, Research and Innovation. ICERI2016 Proceedings. 5607-5618.
[17]. Lorem GF, et al., Ageing and mental health: changes in self-reported health due to physical illness and mental health status with consecutive cross-sectional analyses BMJ Open 2017;7:e013629.
Disease awareness not delivering? Here’s why…
We are all very aware of the healthcare system challenges we face in terms of strained resources and sub-optimal patient outcomes – health inequalities continue to worsen, chronic conditions continue to rise, and cancer survival rates have slowed significantly despite advances in treatment options. This article is NOT going to rehash these challenges or add More…
We are all very aware of the healthcare system challenges we face in terms of strained resources and sub-optimal patient outcomes – health inequalities continue to worsen, chronic conditions continue to rise, and cancer survival rates have slowed significantly despite advances in treatment options. This article is NOT going to rehash these challenges or add further analysis to the extensive body of evidence, but instead explore a small part of the potential solution in the form of behavioural science.
It’s time to step down awareness and embrace the age of activation.
Patient populations that are more involved and invested in their health benefit at the individual, healthcare system, and societal level.1,2 And yet we know that a challenge to disease awareness is often that it sends people into a healthcare system without equipping them to navigate it efficiently. Considered patient activation supports the system by empowering patients with the knowledge, skills, and confidence to optimise their healthcare journey.
We need to understand how to ‘activate’ individuals, what buttons to push to motivate them and nudge them towards health-seeking behaviour.
Evidence and experience suggest that this rarely has anything to do with knowledge about a disease and is often associated with factors such as who’s saying the message, how attention-grabbing the intervention and communications are (the tool or asset itself and the creative identity), and the emotions they’re feeling at the time.3 It requires meaningful and in-depth insights gathering and a comprehensive understanding of human behaviour to identify effective behavioural levers amidst a lot of noise. It is purposeful, targeted and supported by robust evidence.
Disease awareness alone imparts knowledge without necessarily considering behavioural intention and change. It’s putting information out without designing an environment or intervention to ensure a patient engages and does something about it. The intention-behaviour gap4 – the phenomenon where behavioural intention doesn’t translate into action – is well documented in health, and has to be considered through patient activation if we hope to make a measurable difference.
We must prioritise the needs and intention of the audience, adapting communications to what they need to hear to act, anticipating their interpretation and nudging them to execute health-seeking behaviours.
With patients exposed to more messaging and noise than ever before, and with multiple, pressing demands on their attention, communications programmes now need to intelligently cut through, resonate and change behaviour, not just share information.
At Aurora, we use behaviour change frameworks adapted through a suite of tried and tested tools. This ensures we create a holistic picture of our target audience, including how they understand their condition in the context of themselves, medically, and culturally within society, and establishing the factors governing their capability, opportunity and motivation to engage in certain behaviours.
We have the experience and expertise to embrace the messy and complex lives of our audiences, prioritise strategies that work in this environment (not despite it), and use tools to ensure measurable behavioural impact.
We’ve entered an age of patient activation and this cannot be achieved effectively without behavioural science. Equipped with the knowledge, methodologies and motivation to focus on driving real behaviour change, we’ve launched our All for Activation approach.
Demand more from your communications programmes, go beyond awareness for awareness’ sake, and champion targeted ‘activation’ as best practice.
Partner with a team that truly understands human behaviour, can uncover key insights and co-create strategies that drive real, measurable behavioural change and improve outcomes for patients. Awareness can be an effective step on the path towards proactive disease management, but it is not an end in itself. True, targeted patient activation considers the behavioural changes required, and in doing so, changes lives.
If you want to go beyond disease awareness to create meaningful behavioural change, please get in touch: hello@auroracomms.com
- What The Evidence Shows About Patient Activation: Better Health Outcomes And Care Experiences; Fewer Data On Costs. Available at: https://www.healthaffairs.org/doi/10.1377/hlthaff.2012.1061. (Accessed March 2024)
- Patient Engagement: Four Case Studies That Highlight The Potential For Improved Health Outcomes And Reduced Costs. Available at: https://www.healthaffairs.org/doi/abs/10.1377/hlthaff.2014.0375. (Accessed March 2024)
- MINDSPACE: Influencing Behaviour Through Public Policy. Available at: www.bi.team/wp-content/uploads/2015/07/MINDSPACE.pdf. (Accessed March 2024)
- Understanding the Intention-Behaviour Gap. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9386038/ (Accessed March 2024)
International Women’s Day 2024: Inspire Inclusion
The women shaping healthcare communications Here at Aurora, our bright, creative and energetic team represents diverse backgrounds from PhDs to ex-journalists and much in between! This diversity ensures our ability and agility in the ever-changing healthcare landscape. Today, on International Women’s Day 2024, themed ‘Inspire Inclusion’, we shine a spotlight on our barrier-breaking female colleagues, More…
The women shaping healthcare communications
Here at Aurora, our bright, creative and energetic team represents diverse backgrounds from PhDs to ex-journalists and much in between! This diversity ensures our ability and agility in the ever-changing healthcare landscape. Today, on International Women’s Day 2024, themed ‘Inspire Inclusion’, we shine a spotlight on our barrier-breaking female colleagues, whose interests in the sciences have led them to bring their enthusiasm and skills to healthcare communications.
Unreached equality in science
Statistics reported by The Royal Society reveal significant gender disparities in science, with three men for every two women. This could potentially be attributed to a lack of support for women and girls’ scientific interests, resulting in the underrepresentation of women in the sciences. While there’s broad awareness of the need to enhance access for women and girls in science, substantial actions, particularly for marginalised groups, remain insufficient.[1]
With these challenges in mind, it is crucial to recognise and celebrate the achievements of women with scientific interests, supporting an inclusive environment that empowers them to thrive. This sentiment aligns with the spirit of International Women’s Day, a global observance dedicated to acknowledging and advocating for the rights and contributions of women, including in the workplace and in the sciences.
Storytelling and science
Healthcare communications occupies an intersection between science and creativity, serving as a bridge between the technical intricacies of medical advancements and the need for accessible messaging. It is within this dynamic space that the power of scientific storytelling can be harnessed to help transform lives.
For our Scientific Lead, Georgia Hartnell, scientific storytelling is central to her motivation to work in healthcare communications. “Science has the potential to transform lives, but science only becomes truly transformative when it is known by those who need to know it. This underpins my passion for scientific storytelling — distilling complex data into compelling narratives that resonate with patients and clinicians and ultimately motivate change.”
Reflecting on this year’s ‘Inspire Inclusion’ theme, Georgia notes the incredible support she has had from male and female colleagues throughout her career. “For me, ‘Inspire Inclusion’ means mentorship from people who advocate for representation in the workplace. I have been so fortunate to have had access to supportive mentors at every stage of my career, and I hope to be a similar role model for other women in their healthcare communications”.


Leveraging a scientific degree in healthcare communications
As Georgia notes, working in healthcare communications means science is the foundation of everything we do. An interest in the sciences is important to healthcare communications as it provides the basis to navigate complex medical information and communicate it effectively.
For Neshat Islam, Senior Account Executive, transitioning from her degree in Biomedical Science to healthcare communications was a natural progression in her career. “Moving from Biomedical Science to healthcare communications felt like a seamless progression. At Aurora, I bring my understanding and curiosity for disease indications and mechanisms to the research and conversations I undertake daily, while the analytic skills I developed from my degree complement the bigger-picture strategic work we complete for our clients.”
In her role at Aurora, Neshat believes in embodying the values of ‘Inspire Inclusion’ every day. “I strongly believe in the importance of women’s representation in the workplace, and I feel extremely fortunate to be surrounded by like-minded colleagues who make me feel supported and valued. Through my work, I have the opportunity to actively contribute and observe other women breaking down barriers in the workplace.”
Utilising behavioural science
While Neshat has been fortunate to receive encouragement throughout her academic and professional experiences, we know that this is sadly not the case for everyone. The recent UK Parliament Inquiry into Diversity and Inclusion in the sciences highlights the underrepresentation of women, certain ethnic minorities, people with disabilities and those from disadvantaged backgrounds. Learned behaviours and unconscious bias play a pivotal role in the low participation of girls in science subjects, as stereotypes like “science subjects are meant for boys” discourage their involvement. Behavioural insights have been applied to address this challenge, with the UK Government achieving positive outcomes through targeted efforts to increase girl students’ uptake of science subjects at A-Level.
Last year, Molly Stephenson, Senior Account Director and our resident behavioural expert, attended the Nudgestock behavioural science festival, where she heard from Mary Ann Sieghart on ‘Fighting the authority gap.’ This discussion delved into the impact of bias on behaviour and performance, or ‘stereotype threats,’ which affect women personally, academically and professionally.
Molly reflects, “I loved hearing from Mary in her book, The Authority Gap, she describes why and how women are still taken less seriously than men and what we can do about it. A key takeaway is the indisputable impact of representation in making these shifts toward better circumstances for women and the benefits for everyone in society when this happens.”
Further emphasising the importance of representation in bringing about the necessary changes for women in the workplace and beyond, Molly notes, “With representation having profound impact on our own judgments of our self-worth and capabilities, I’m grateful to work for an agency that recognises and embraces the positive impact of gender diversity in leadership.”


Being the change we want to see
At Aurora, we aspire to be a representation of an agency where women in science are not only encouraged but valued. While there is still work to be done, we are committed to championing women in their development as future leaders in health communications and improving diversity across our industry and the wider healthcare landscape. And finally, we take pride in collaborating with clients who ‘Inspire Inclusion’.
Our CEO Claire Eldridge said “We’re really proud of our commitment to excellent science that underpins all the amazing work we do for our clients. We’re especially proud of our wonderful, representative team that delivers on this commitment every day.”
Here’s to our incredible team who all work to ‘Inspire Inclusion’ every day!
[1] It’s important to note that The Royal Society’s publication did not cover data on non-binary individuals in the sciences.
A new way of thinking about patient activation
We’re delighted to launch All for Activation, Aurora’s new behavioural science approach for patient activation. Our new approach aims to create more equitable and sustainable management of chronic illnesses. Chronic illnesses are a leading cause of mortality and morbidity, and account for a large majority of healthcare costs. As populations continue to age, the incidence More…
We’re delighted to launch All for Activation, Aurora’s new behavioural science approach for patient activation. Our new approach aims to create more equitable and sustainable management of chronic illnesses.
Chronic illnesses are a leading cause of mortality and morbidity, and account for a large majority of healthcare costs. As populations continue to age, the incidence of chronic illnesses will grow. To improve patient outcomes and reduce the economic burden associated with chronic illnesses, a greater focus on prevention, early intervention and proactive self-management is needed, including patient activation strategies.
We believe that the pharmaceutical industry, with its resources and networks, can be a catalyst to drive broader adoption of patient activation in Europe. Key to success is working in partnership with the patient and clinical community to co-create impactful activation programmes that go beyond patient engagement – and Aurora is here to uncover the opportunities and co-design best practice capable of shaping policy, transforming dynamics, and fostering behavioural changes.
Our team includes experts in patient advocacy, behavioural science and communications. We have been listening to patients and working with existing clients and experts to shape our approach, as well as understanding intervention techniques and best practice tools such as the Patient Activation Measure which brings rigour to decision making and measurement.
What is patient activation and why is it important?
Patient activation is focused on an individual’s willingness and ability to take independent actions to manage their health and care.1 It equips people with the knowledge, skills and confidence to improve health literacy, participate in shared decision making and effectively self-manage their conditions.
At Aurora, we believe that for patient activation to thrive, it requires not only a shift in mindset and behaviour from patients, but for everyone involved in the health of an individual to champion and support patient activation. That’s why we are starting to drive the use of the term “health activation” as responsibility to adjust behaviour should not sit solely with patients. We believe that while emphasising a patients’ willingness and ability to take action is critical, the support of healthcare professionals is also vital to achieve long-term success.
To make health activation a sustainable part of chronic illness management strategies, we need to consider the capability, opportunity and motivation of everyone involved, including policy makers, patient advocacy groups, healthcare professionals, as well as patients and caregivers.
Why should stakeholders take the time to invest valuable time, energy and resources in health activation?
Because health activation means individuals have greater ability to pursue the treatment that’s right for them, leading to better health outcomes and better economic outcomes for the healthcare system.2,3
Guided by our PARTNER principles and behavioural science models, our new approach goes further to change behaviours. Our team possesses the expertise and experience to help companies collaborate with the patient community to deliver impactful, measurable activation programmes.
If you are working in a chronic illness therapeutic area and looking to go beyond disease awareness to create meaningful change in partnership with the patient community, please get in touch to discuss our new All for Activation patient activation approach: Rosanna.forrest@auroracomms.com
2023 – A landmark year for Aurora
In 2023, Aurora achieved monumental milestones, our year was a perfect blend of hard work and celebration. We have a lot to be proud of, and have worked hard to set ourselves up for our continued growth journey through our new positioning that resonates through our entire team. Explore the highlights of our extraordinary 2023. More…
In 2023, Aurora achieved monumental milestones, our year was a perfect blend of hard work and celebration. We have a lot to be proud of, and have worked hard to set ourselves up for our continued growth journey through our new positioning that resonates through our entire team.
Explore the highlights of our extraordinary 2023.
This year we:
Won 17 new clients
Launched 11 client campaigns
Fought health and social injustice in 30 disease areas
Made waves at 9 congresses
Moved home
Went on holiday together
We worked hard…
And played hard.
Redefining medical communications in the age of omnichannel engagement
Medical affairs has undergone a subtle but profound transformation that has led to a need for cross functional collaboration across medical, market access, commercial, and patient engagement, to name a few functions. There are three trends underlying this transformation: The increased complexity in the new medicines landscape The adoption of digital engagement The advent of More…
Medical affairs has undergone a subtle but profound transformation that has led to a need for cross functional collaboration across medical, market access, commercial, and patient engagement, to name a few functions. There are three trends underlying this transformation:
- The increased complexity in the new medicines landscape
- The adoption of digital engagement
- The advent of omnichannel communications
What omnichannel is, as well as how to map out and execute an omnichannel journey, is subject to various definitions. We define omnichannel engagement as a seamless, personalised experience with integrated customer touchpoints, where the data metrics for how content has been delivered and received are available and synchronised across all available channels. In contrast, a multichannel experience offers multiple, single journey touchpoints that are not synchronised and create a disconnected customer experience.
Demand by healthcare professionals (HCPs) for medical information that is readily available, relevant, and conveniently found in their preferred channels has accelerated the adoption of digital and the need for omnichannel engagement in medical affairs. As such, pharmaceutical and medical device companies have met the demand for new content with an increase in investment and allocation of resources to digital and omnichannel activities. Interestingly, despite the effort, surveys of both pharmaceutical employees and HCPs revealed that two-thirds of pharmaceutical responders were dissatisfied with their current omnichannel activities.[1] Similarly, two-thirds of HCPs felt they were ‘spammed’ with digital content.[2] Such insights beg the question. Where is the disconnect is between what HCPs want and what they get?
A likely reason for this generalised dissatisfaction is that, in most cases, HCPs are experiencing disconnected journeys where each touchpoint keeps repeating the same message without expanding or enriching their awareness or education.
That HCPs feel spammed suggests that most content reaching them is either irrelevant to their interests or simply repetitive. Further research into the interests of HCPs show, unsurprisingly, that they seek out information on treatment advances, clinical trial data and clinical research.[3] However, they have less time to keep up to date and prefer ‘bite-size’ content on digital or mobile channels, available at a time convenient to their schedule. Therefore, the key to greater engagement and greater impact can be defined as:
- Novelty: The number one reason HCPs engage with communications from pharma
- Specificity: HCPs prefer communications with clear, specific language, information, and terms to help them gauge how relevant the information is to them
- Convenience: Technology that reduces effort and anticipates HCP needs
- Digestibility: Communications that quickly address the information need
To remain relevant, traditional medical content must continually evolve into intelligent content, which can be structured into approved, format-agnostic, core fragments and assembled into various materials that can be used across an omnichannel journey. In our experience, our clients’ biggest challenge in omnichannel planning is mapping out and executing an omnichannel delivery plan that intelligently takes account of the potential touchpoints and possible variable interactions (in effect, a decision tree) while remaining relevant, engaging, and code-compliant.
To achieve the latter, first, we must define our engagement objectives and their relation to any broader strategy we have in place. Only then can we identify the tactics and channels needed to meet the audience and goals across the customer journeys. Essential to this plan is a deep understanding of customer segments and/or personas (detailed stakeholder mapping) to ensure that personalised content is delivered to the right customer at the right time. The omnichannel delivery plan then becomes the visualisation of the customer journey with the key customer interactions with intelligent content developed for the specific persona.
At Aurora, our approach to medical communications means our specialist teams can be brought in to assess and recommend the strategy, approaches, tools and measurement needed to transition from disappointing multichannel journeys to effective omnichannel engagement. Our specialist-driven approach to omnichannel engagement can help with:
- Innovation: Omnichannel maturity assessment before execution
- Strategy: Ensure a correct approach based on the company’s and the brand’s strategic drivers as well as the market landscape
- Medical communications: Develop intelligent content informed by customer-specific personas
- Digital: Upskilling of internal teams, technology and platform assessment, and execution of the omnichannel roadmap
Aurora is an independent, integrated healthcare communications and marketing agency committed to improving lives by accelerating access to medical innovation. With seamless access to senior leaders and an unwavering commitment to agile delivery, we foster collaborative partnerships.
Unlock the power of effective omnichannel engagement for your clinical trial recruitment strategy with Aurora’s specialist-driven approach – reach out to Chris Hall, Strategy Director at chris.hall@auroracomms.com and elevate your medical communications today.
[1] Across Health; Multichannel Maturometer 2021
[2] Accenture: The “new” rules of engagement: How pharmaceutical companies can give HCPs the new and meaningful interactions they want
[3] Nature publishing. Available at https://partnerships.nature.com/blog/creating-content-to-engage-health-professionals/ (Accessed Aug 2023)
Speaking up against health inequalities: the role of communications

Health inequalities are avoidable, unjust and systematic differences in health between different groups of people.1 They are a complex and growing issue, impacting individuals across the globe at all stages of the health journey. It is not a small nor straightforward topic. Health inequalities involve a range of differences in health measures, including health status and More…
Health inequalities are avoidable, unjust and systematic differences in health between different groups of people.1 They are a complex and growing issue, impacting individuals across the globe at all stages of the health journey.
It is not a small nor straightforward topic. Health inequalities involve a range of differences in health measures, including health status and access to and experience of healthcare. Disparities in these experiences are often dictated by differences in an individual’s or group’s wider determinants of health. These include a diverse range of social and economic factors such as income, housing and education, but also an individual’s attitude towards, and trust of, the healthcare system.
At Aurora, we are on an ongoing journey to better understand health inequalities, their causes and the impacts they have. As an agency, we are committed to identifying and actioning what we can do, together with our clients and partners, to help tackle the issue.
Getting the data right
Data is vital for driving actionable insights and identifying solutions to health inequality challenges. We need data to understand the root causes of the issues, and to direct the focus of interventions and solutions. However, when it comes to data, we must focus on quality rather than quantity and ensure that data collection around protected characteristics, such as race, disability and sexual orientation, is not forgotten about or deprioritised.
The balance must be right between collecting valid, insightful data, and taking solution-focused action. We must not fall into the trap of ‘analysis paralysis’ and instead ensure we have the confidence to communicate and act on the insights we gather.
This is a challenge that NHS leadership are facing, with crucial projects and interventions such as the NHS Workforce Plan being delayed due to ongoing analysis and repeated reconsiderations at a national level.2
The role of health literacy
Health literacy refers to having the appropriate skills, knowledge, understanding and confidence to access, evaluate and use health information and services.3 It is fundamental to achieving health equality and needs to be carefully considered when developing health materials, resources and communications for patients.
The average reading age across the UK is 9-11 years, yet health information and resources often don’t reflect this. It is estimated that 42% of working-age adults in England are unable to understand and make use of everyday health information.3
A bottom-up approach
Collaboration is key. We need to be united in our approach to tackling health inequalities and work collectively with partners across the healthcare landscape when setting strategic vision with our clients. Not only is collaboration with patients essential, but alliance with communities, health services and third parties is vital to enable innovative solutions and to drive change.
Building trust with communities is fundamental to facilitate engagement. The ask from the community needs to be clear, ensuring that the right language and appropriate channels are used to reach these audiences.
How can we drive change within communications
With a topic as vast as health inequalities, we have of course only scratched the surface. It is a topic that we at Aurora feel passionately about and will continue to work with our clients towards a systematic and sustained approach to drive change. To do this, we need to consider:
- As communicators, we know talking about the problem can only do so much. We need to be adopting a behaviour change mindset to find tangible solutions relating to the modifiable risk factors of health
- It is vital that we are listening to the voices of individuals with lived experience. As a communications agency, we have a responsibility to involve patients and people with lived experience when developing health communications and resources to ensure that they are ‘fit for purpose’ and sensitive to the literacy and needs of their relevant audiences. Partnering with voluntary, community and social enterprises (VCSEs) and grassroot organisations is crucial to understand the needs of communities when developing interventions. These organisations need to be brought in from the very start and not just to test the credibility of something already developed
- Action required to bring about change is universal and will take time. We, and the clients we partner with, have a responsibility to ensure reducing health inequalities runs through the everyday work that we do, to share learnings and to not be afraid to adapt practices as we go
If you’d like to find out more about our work in reducing health inequalities, behaviour change, patient engagement or the other strategic practices we offer at Aurora, get in touch at hello@auroracomms.com
References
- The Kings Fund. What are Health Inequalities? Available at https://www.kingsfund.org.uk/publications/what-are-health-inequalities. Last accessed July 2023.
- UK Parliament. Latest NHS reforms will not succeed until Government fixes longstanding problems. Available at https://committees.parliament.uk/committee/127/public-accounts-committee/news/185951/latest-nhs-reforms-will-not-succeed-until-government-fixes-longstanding-problems/. Last accessed July 2023.
- Public Health England. Local action on health inequalities. Improving health literacy to reduce health inequalities. Available at https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/460710/4b_Health_Literacy-Briefing.pdf Last accessed July 2023.
Moving beyond vanilla to improve patient diversity in clinical trials

Enabling greater patient diversity in the development of medicines is a clear priority for our industry as regulators become increasingly concerned by the uneven reflection of population demographics in study samples. In a 2020 analysis of global participation in clinical trials, the FDA highlighted major discrepancies between trial participants and the global population. Of 292,537 More…
Enabling greater patient diversity in the development of medicines is a clear priority for our industry as regulators become increasingly concerned by the uneven reflection of population demographics in study samples.
In a 2020 analysis of global participation in clinical trials, the FDA highlighted major discrepancies between trial participants and the global population. Of 292,537 participants, 76% were white, 11% were Asian and only 7% were Black.[1] In comparison, three quarters of the global population is comprised of Asians and Africans alone.
No silver bullet
It is a complex matter with no silver bullet solution. Instead, a concerted effort from all stakeholders is needed, including regulators, healthcare providers, patient and community organisations, the pharmaceutical industry and policy makers.
However, there are some straightforward patient-focused solutions that can be executed, which can make a significant difference.
In many clinical trial recruitment strategies, we often see a somewhat vanilla design, lacking sufficient consideration for the diverse populations they need to engage.
Deep patient connection
We know from experience that strategies co-designed in partnership with patients – and fuelled by insight from all target demographics – are more successful. They enable us to create a deep connection with each patient population, reflecting their experience – physical, emotional and information seeking.
Our unique approach starts with an insights-led patient experience mapping exercise to identify the required participant profiles; what they will wish to gain and avoid from participation; the points in their experience when they are most likely to participate; and the channels and tactics to best reach and engage them.
We then work with patients who fit the identified profiles to co-design all trial materials globally, and take it a step further at a country level, testing globally designed strategies and materials with local patient audiences.
When a patient-focus is embedded in the way we think and work – from the very first planning meeting right through to study completion, we are more likely achieve representative study populations, ultimately leading to better treatments.
[1] U.S. Food & Drug Administration. 2015–2019 drug trials snapshots summary report. FDA https://www.fda.gov/media/143592/download.
If you want to find out more about how we can help accelerate your clinical trial recruitment strategy, please reach out to Stephen O’Farrell (stephen.ofarrell@auroracomms.com) who is Head of Patient Engagement at Aurora Healthcare Communications.
Hard to reach: culture, diversity and voices

We attended the Patient Centricity and Engagement conference earlier this year to hear from the leading pharmaceutical companies on how they are striving for patient centricity. Diversifying the voices heard We heard from several companies about how they are trying to diversify their patient panels who provide guidance across various projects, such as disease awareness More…
We attended the Patient Centricity and Engagement conference earlier this year to hear from the leading pharmaceutical companies on how they are striving for patient centricity.
Diversifying the voices heard
We heard from several companies about how they are trying to diversify their patient panels who provide guidance across various projects, such as disease awareness or clinical trial recruitment. While patient panels are becoming more and more common, the absence of diversity means there is a distinct lack of varied viewpoints and experiences.
One pharmaceutical company have looked to navigate this challenge by leveraging social media to source contributors for its country insights panel, meaning more people hear about the opportunity to share their lived experience. They are now on their way to creating a virtual insights panel that has contributors from across the UK and from differing cultural, socioeconomic, and religious backgrounds.
Another company shared how they are finding it challenging to reach those who don’t tend to engage with the patient groups as this is their main route to speaking with the patient community. However, a patient representative outlined that while seeking those who are ‘hard to reach’, the voices of those who are engaged need to talk loudly for those who are suffering quietly. Engaging with those people in the first instance will ensure programmes can be successful and iterations can be made once more of the population become engaged.
It’s not just patients who are ‘hard to reach’
Instilling patient-centric approaches within teams and across a whole organisation requires a behaviour and mindset change. While many companies talk about being patient-centric, we heard that engaging cross-functional colleagues in patient engagement or activation programmes can be difficult and a cultural shift is needed which takes time.
The companies that saw successful patient engagement projects launched shared that they had key ambassadors for patient-centric work outside of the patient relations team and they were included in cross-functional working for programmes, whether it was in medical, compliance or marketing. These key ambassadors continuing to talk actively about involving patients and interrogate projects to ensure patient experience and guidance has been sought meant that other brand teams were then considering approaching patient programmes in a more dynamic and holistic way.
Driving change with patients and organisations
The conference left us with three main areas for reflection. To drive change and engage those who are ‘hard to reach’, we need to consider:
- Organisational culture and structure take time to change, however it is important that patient engagement runs through the heart of companies, and those that are hesitant are brought along on the journey
- People living with the conditions should set the agenda and drive conversations – if a diverse group of patients aren’t included in the co-creation of patient engagement programmes, then the programme is unlikely to create change for, or activate, the target population
- To reach those who are deemed to be ‘hard to reach’, whether it’s patients or within an organisation, ambassadors and louder voices need to speak up, create the initial change and bring the less-engaged along on the journey with them
If you’d like to find out more, look at our strategic practices – we can help you improve lives and prove it. Get in touch today!
Reaching the Hard to Reach
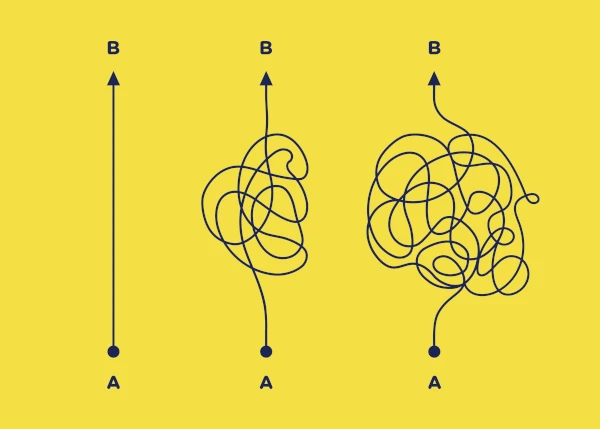
The phrase ‘hard to reach’ feels simultaneously like a clear description of a marginalised community and an imprecise attempt at grouping millions of people. In a recent industry webinar, reaching ‘hard to reach’ patients was described as “the holy grail” and is one of the next great challenges for those working in healthcare. So, what More…
The phrase ‘hard to reach’ feels simultaneously like a clear description of a marginalised community and an imprecise attempt at grouping millions of people. In a recent industry webinar, reaching ‘hard to reach’ patients was described as “the holy grail” and is one of the next great challenges for those working in healthcare.
So, what is ‘hard to reach’?
We will be exploring what ‘hard to reach’ means for different audiences throughout 2022. While there isn’t a set industry definition of ‘hard to reach’, some groups of people come up time and again as those who do not actively engage with the content we produce. However, ‘hard to reach’ isn’t just about the patients; the term could also be used to talk about healthcare professionals or even teams within pharmaceutical companies.
Our experience with ‘hard to reach’ groups
Over 17 years, we have, in many cases more by luck than judgement, ended up trying to understand how we engage and activate a specific ‘hard to reach’ audience, including:
- Raising awareness and understanding of symptoms in people who are potentially living with complex underdiagnosed rare diseases
- Improving engagement in symptom control in people living with common, previously considered fatal diseases
- Engagement of healthcare professionals in the differential diagnosis of diseases so rare, they may only see one case in their career
- Allowing peer-to-peer support for patients living with rare diseases who may never have spoken to someone else living with that condition
- Creating engagement across internal audiences when complex and challenging business decisions need to be made
This breadth of work has given us extensive experience in changing systems, increasing engagement, and ultimately changing people’s lives who were previously unengaged in a specific problem. But we know the problem is much bigger than this.
Whatever we want to call it or however we want to categorise these groups is not that important. Fundamentally, engaging ‘hard to reach’ audiences is about equity. Be that in diagnosis time, treatment access or decision making. We are trying to ensure equity for everyone living with a specific disease or condition to live their best life.
Over the coming months, we will be discussing more on reaching, engaging, and activating specific ‘hard to reach’ audiences. We will even begin to explore some new definitions that have helped us define how to best support these groups (or those trying to reach them). For now, we’ll leave with one final thought: what is it about these groups that make them ‘hard to reach?’
If you’d like to find out more, look at our four strategic practices – we can help you improve lives and prove it. Get in touch today!
Re_framing the future

Our blog has been quiet of late, but that’s been deliberate. Mainly because we’ve had a great start to the year and our team has been busy delivering for our clients, but also because we’ve been working on practising what we preach. Connecting what we do with why we do it – and for us More…
Our blog has been quiet of late, but that’s been deliberate. Mainly because we’ve had a great start to the year and our team has been busy delivering for our clients, but also because we’ve been working on practising what we preach. Connecting what we do with why we do it – and for us all it’s to help people access healthcare, access innovation and improve lives.
To help us better understand how we do that, we’re launching “Aurora: re_frame the future”. A thought leadership platform where we will explore the biggest challenges, trends and directions of travel in healthcare amongst some of the brightest individuals in the industry. From global NGO leaders to health think tanks, KOLs, patient groups and patients themselves, we are seeking to connect with those that are shaping the future of our industry, those who are having a profound impact upon it, so that we can draw evidenced insights around where are industry is moving towards, and moreover… why it is moving there.
Our first interview is with Raquel Peck, patient advocacy specialist, chair of the International Experience Exchange of Patient Organisations, consultant with World Health Organization and ex-CEO of the World Hepatitis Alliance. We will explore some of the latest trends in collaboration between pharma and patient groups, priorities in achieving the 2030 Sustainable Development Goals (SDGs), how 2022 is shaping up to be a pivotal year in driving health policy change towards a more humanised healthcare ecosystem. Sound good? We hope so, and can’t wait for you to join us. Keep an eye on our social channels for details shortly. Our team will be sharing many more of these insights-based interviews over the next few months.
Launching Aurora Social Impact
So, less about the future for a second, what about today?
An organisation’s commitment to social purpose matters more than ever to its customers, employees, and communities. In keeping with the principles of the 2030 SDGs, we want to do everything we can to ensure that no-one is left behind when it comes to accessing healthcare. Globally, regionally and nationally, we can all play a role through the work that we do to address social inequity in healthcare. We have eight years left to achieve the sustainable development goals, so the hard work starts today, and our clients can have a direct impact on us reaching them in time.
Specifically, we as communicators can also advocate and enhance collaboration efforts between patient organisations, pharma, and academic institutions. We can move beyond simple disease awareness messages to design campaigns that engage harder to reach communities and address societal inequalities in accessing healthcare and treatments. COVID has shone a stark light on how much there is still left to achieve in addressing universal health coverage: the conversation has changed.
To help our clients do just that, we have launched Aurora Social Impact. A practice where we combine our expertise in measurement and campaigns, with our heritage in storytelling, to help pharma, biotech and NGOs create social impact and address social inequity in healthcare. We’re doing this with two major clients in diabetes and oncology and we will now be expanding the offer as a dedicated business practice.
Get in touch
There’s no doubt that right across the healthcare industry, 2022 is shaping up to be a pivotal year, with renewed focus on the SDGs, in particular. The right to health is a fundamental human right and we’re excited to be looking at more opportunities to work with clients in helping make sure this right is realised.
If you want to hear more then get in touch. Let’s get to work.
Creating “metahealth” in the metaverse

In late October, Facebook changed the name of its holding company to Meta to stake its claim on the concept of the metaverse, deemed to be the future of the internet. Described on the company website as “the next evolution in a long line of social technologies”, the announcement has, rightly, also been perceived by More…
In late October, Facebook changed the name of its holding company to Meta to stake its claim on the concept of the metaverse, deemed to be the future of the internet. Described on the company website as “the next evolution in a long line of social technologies”, the announcement has, rightly, also been perceived by industry commentators as an attempt by Facebook to distract from its current troubles with the rebrand.
Defined as “a set of virtual spaces where you can create and explore with other people who aren’t in the same physical space as you”, the potential of the metaverse could be seen as positive, particularly in a world where working from home and the expectation of on-demand services become more common. Yet stepping away even further from true reality, particularly with the recent learnings around the unprecedented impact of social media on mental health, the concept raises big questions including who monitors a seemingly endless digital world for corruption, abuse, distorted ethics, and data breaches.
What does the metaverse mean for healthcare?
With telehealth, remote appointments with HCPs and digital solutions for health services becoming more common, spurred on by the pandemic, users have begun to feel more confident in moving away from the traditional person-to-person relationships when it comes to healthcare.
The metaverse could unlock further opportunities as outlined in Forbes: “[the metaverse] has significant potential applications in the realm of healthcare. Some very basic examples include: remote monitoring of patients that require critical care; better data and insights into clinical outcomes (e.g. blood sugar monitoring, heart rhythm tracking, etc.); augmented tracking of physical health, virtually.” In the UK, reducing the need for hospital visits and treatment, when appropriate, is essential to aid the NHS’ recovery following the impact of COVID-19.
Yet there is a key barrier to ensuring the metaverse, and its potential benefits, is available to everyone around the world – universal digital infrastructure.
The digital divide
According to research conducted in early 2021, there were 4.66 billion active internet users worldwide or 59.5% of the global population, meaning roughly 40% of the world’s total population remain offline. A huge number of people are already on the wrong side of the digital divide that the metaverse will only amplify. From a global health perspective, as organisations simultaneously work towards achieving the 2030 Sustainable Development Goals for universal healthcare coverage, with the ethos ‘leave no one behind’, then the digital divide presents a huge barrier that can only be exacerbated by movements toward the metaverse.
For there to be a true “Metahealth”, all aspects of country specific, regional and global healthcare ecosystems will need to undergo an intense digital transformation and a disruption in processes, workflows, practices and delivery methods will need to take place. While this is happening, addressing inequalities in the current standards of care and making healthcare accessible to those patients who are deemed marginal or hard to reach (defined as those who cannot be reached by traditional and conventional methods for any reason) needs to be the top priority of the healthcare industry.
So how can pharmaceutical companies increase health access while embracing digital innovations?
The metaverse, as claimed by Facebook, is still in the early stages and may take a decade to evolve, bringing with it immense potential in terms of healthcare. Whilst the metaverse is evolving, it’s easy to see the trail of innovation in its wake that is available to pharma now, including virtual reality (VR) and artificial intelligence (AI). Medtech companies are already investing with platforms available for healthcare professionals, bringing them together for simultaneous education, training and planning as well as collaborative medical procedure.
However, while digital platforms are increasing health equity and access in many ways, pharmaceutical companies must continue to work with patients, both online and offline, from diverse backgrounds to define and co-create the way research, drug development, clinical trials and care take place. The ultimate goal should be to close the health inequality gap and bridge the digital divide now, before either widens, so that when the metaverse reaches maturity it can have a significant impact on patients around the world.
Three ways pharmaceutical companies could be closing this gap through Corporate Social Responsibility now, are:
- Investing in improved access to the internet for communities where lack of digital infrastructure is impacting access to healthcare services and information
- Improving digital literacy for potentially marginalised groups through community and school partnerships
- Increasing access to information, either online or offline, to encourage engagement with conditions, symptoms and self-management of health. For example:
- Online: ensuring all websites meet Web Content Accessibility Guidelines (WCAG 2.1)
- Offline: provide information in a variety of offline formats that HCPs can access and provide to patients who cannot access them digitally
At Aurora, we are working with clients to identify the best way to access hard-to-reach patients across different disease areas and navigate barriers that may be holding patients back from accessing the care they need to live healthy lives. If you’d like to hear more or have a challenge you would like to discuss, please contact the patient engagement practice: hello@auroracomms.com
GLOBALHealthPR Launches New Identity as Global Health Marketing & Communications
Today, GLOBALHealthPR, the world’s largest and most robust network of independent healthcare agencies, announced it has rebranded as Global Health Marketing & Communications (GHMC). After over two decades in operation, GHMC’s new identity reflects an evolution and expansion of communications and marketing capabilities in recent years driven by the increasingly integrated and constantly changing media landscape. More…
Today, GLOBALHealthPR, the world’s largest and most robust network of independent healthcare agencies, announced it has rebranded as Global Health Marketing & Communications (GHMC).
After over two decades in operation, GHMC’s new identity reflects an evolution and expansion of communications and marketing capabilities in recent years driven by the increasingly integrated and constantly changing media landscape. The GHMC brand emphasizes the meaningful human connections that improve health outcomes for all through the delivery of dynamic, health-lingual experiences globally, regionally and locally.
Aurora is the exclusive UK partner and European hub for GHMC and we have delivered strategic campaigns in close partnership with the network for more than 14 years. We are excited for this new chapter as GHMC which elevates our identity to be fully representative of the extensive, health-specialist services being offered.
Aurora has a broad set of communications capabilities ranging from patient engagement to societal impact, embodying the network’s mission to help clients radically improve health outcomes for all. We were recently shortlisted in the Global Content category for the PRWeek Global Awards for our work on the global programme SMA My Way, for which we collaborated with the spinal muscular atrophy community and Roche.
If you would like to hear more about GHMC, our role within the network or our wider capabilities, please do get in touch.
International Women’s Day: Reaching the hard to reach in Madagascar

This International Women’s Day we want to shine a light on one of the many amazing women here at Aurora. Following her Master’s, Anna Lenherr brought her passion for addressing health inequality from the field to Farringdon, where she now works as an Account Executive. Read on to learn more about her inspirational experiences providing community support More…
This International Women’s Day we want to shine a light on one of the many amazing women here at Aurora. Following her Master’s, Anna Lenherr brought her passion for addressing health inequality from the field to Farringdon, where she now works as an Account Executive. Read on to learn more about her inspirational experiences providing community support and researching schistosomiasis in Marolambo, Madagascar.
Schistosomiasis is a neglected tropical disease (NTD) caused by parasitic worms transmitted through freshwater snails. The World Health Organization (WHO) estimates this diseases impacts 252 million people globally, with at least 90% of those requiring treatment for schistosomiasis living in sub-Saharan Africa. This disease especially affects poor communities without access to safe drinking water and adequate sanitation. As there is currently no vaccine, the main control methods include preventative chemotherapy treatment through regular mass drug administration (MDA), snail control and health education to raise awareness and understanding of disease transmission and to improve MDA uptake.
While completing a Master’s in International Public Health (MPH) at Liverpool School of Tropical Medicine, I joined Madagascar Medical Expeditions (MadEx), a research project and charity formed in 2014 by medical students at the University of Manchester. The main goal of MadEx is to reduce the burden of schistosomiasis and other neglected tropical diseases in Marolambo, a remote rainforest district in southeast Madagascar. Through collaborations with the Madagascar Ministry of Health and the Durrell Wildlife Conservation Trust, MadEx has run annual expeditions to research disease prevalence, implement a novel health education program in local schools, and advocate for consistent MDA. As part of my dissertation that is currently undergoing publication, I undertook statistical analysis of previous MadEx data to evaluate the association between malnutrition and four years of annual mass praziquantel treatment for schistosomiasis in school-aged children in the Marolambo district.
After graduating, I had the opportunity to join the MadEx 2022 June expedition. Along with a team of three British doctors, two Malagasy doctors and two Malagasy social workers, I flew to Marolambo, Madagascar. Below are the main aims and outcomes of our expedition:
- Hold a ‘Schistosomiasis Teaching Day’ in Marolambo to feedback results of previous expedition research to build and sustain trust among community
- Introduce a novel Schistosomiasis Education Programme (SEP) to local teachers and district leaders and implement this in the local school curriculum in six schools in the Marolambo district
- Carry out quantitative Knowledge, Attitude and Practices (KAP) surveys with school children to investigate any changes from previous years and the benefits of health education
- Conduct qualitative focus group sessions with local teachers and village leaders to further inform the specific needs of the community
- Ensure the sustainability of MadEx by handing over leadership to the Malagasy MadEx team
Reflecting on the successful month of unique challenges to implement a novel health education programme with MadEx, it was hugely insightful to work with a community who are often neglected from large national health campaigns. Engaging with those living in any ‘hard to reach’ population often requires in-person conversations to truly understand their needs.

Since then, I’ve had the opportunity to apply the knowledge and skills I gained from this expedition to the patient-centric work I continue to support at Aurora, from vaccine rollout strategy to health inequality campaigns.
Click here to find out more about how we can help you develop patient-focused projects and campaigns.
New member of an exclusive club – 10 years at Aurora

Dedicating 10 years of our lives to anything takes a great deal of commitment but working for one healthcare agency for a decade is a true achievement that not many of us reach. This year, Rachel Terry, our Editorial Lead, entered a rare club for those of us in the agency world and reached double-digits More…
Dedicating 10 years of our lives to anything takes a great deal of commitment but working for one healthcare agency for a decade is a true achievement that not many of us reach. This year, Rachel Terry, our Editorial Lead, entered a rare club for those of us in the agency world and reached double-digits at one team. We are proud that she reached this milestone with us so we wanted to take the time and discuss her decade at Aurora.
What made Aurora the right agency for you 10 years ago?
Surprisingly, I first joined Aurora as a freelance account manager after being made redundant by my previous agency a few weeks before Christmas. I had held Director roles at various healthcare agencies and thought my account manager days were long behind me, but I had time, the project was interesting and Aurora seemed like a great place to work, so I went for it.
To this day I’m so happy I did, as the situation changed very quickly with the owners, Claire Eldridge and Neil Crump, offering me a permanent Director role within two months.
Due to Aurora’s culture and values, it creates an environment that thrives on entrepreneurial people who are 100% focused on healthcare, where everyone wants to do great work for like-minded clients working on fantastic innovations, doing what we can to make sure they reach the patients that need them.
Why is Aurora still the right agency 10 years on?
The main thing that has kept me here in the long-term is our culture. I think we’ve got a lovely culture at Aurora where people are encouraged to take the initiative and are also hugely supportive of each other. There is absolutely no office politics, no cliques, no game-playing – as I am not a political person, that makes for a productive, kind and rewarding working environment.
I am not at the stage of my career where I am chasing job titles and the biggest salary package – although they are pretty good at Aurora too – for me the other things are so much more important. It’s about how happy I am and how I can do my best work.
Do you think the difference at Aurora stems from the fact that the founders are still involved on a day-to-day basis?
For many years, Aurora’s independence was a major factor. In terms of our culture, nothing has changed with Aurora’s sale to Spectrum, our long-term US partner in the Global Health Medical Communications (GHMC) network. Claire and Neil, who had the original vision for Aurora and stayed true to it over the years, are still involved (albeit in a shiny new role for Neil), and we continue to focus on making the right decisions based on the needs of our clients and team, because that is essential for sustained business growth in the long-term.
When I wanted to make a change to my role a couple of years ago, I had the opportunity to work with Claire to shape it. This means I now focus on the things I love and enjoy and spend less time doing the things that – after more than 30 years in the industry – I just didn’t want to continue in this later stage of my career. Being able to have that discussion in a really open and honest way was invaluable.
What are you most proud of during your decade at the agency?
When I joined in 2012, Aurora wasn’t particularly focused on awards. I’ve always felt that awards matter to both client and agency teams and was able to make the case that we should enter, even though they create a lot of work. I am proud that we entered the Communiqué Award for Best Small Consultancy for the first time that year and won, and went on to win Consultancy of the Year the following year.
I believe that winning those awards made a difference to how Aurora was perceived by clients and the wider industry. I am also proud that, almost a decade later, we were again a finalist in the Consultancy of the Year category, acknowledging the brilliant work done by the whole team last year, despite the challenges of the pandemic.
What does Aurora need to do to encourage other people to stay for a decade or more?
There are things we need to maintain, and the company culture is definitely one of them. From an employee point of view, I think the culture we have built is exceptional in that it is both entrepreneurial and highly supportive, so it’s a great place to build a career.
Beyond that, I think people need opportunities to grow into new roles, and this process will accelerate with Spectrum’s investment for growth. Some will want to follow the traditional account management/agency management path, but others will prefer to build their career by specialising in new areas. Just as the rise of digital and social opened up opportunities for communicators and agencies to develop new expertise, emerging trends and technologies will create future opportunities not only for people to specialise, but also for Aurora to extend our range of services.
Ensuring people have new challenges and opportunities to develop new skillsets to build their careers in a direction that is right both for them and for the agency is key for longevity – alongside maintaining our great culture and competitive salary/benefits packages, of course!
11 friends, 600km, 360 donations…in memory of one person
Recently, myself and ten other friends took on the challenge of cycling from London (St Albans for me) to Amsterdam, to raise money for Young Lives vs Cancer, all in memory of our good friend Matthew who passed away ten years ago. The cycle covered roughly 600km, went through four countries (England, France, Belgium and More…
Recently, myself and ten other friends took on the challenge of cycling from London (St Albans for me) to Amsterdam, to raise money for Young Lives vs Cancer, all in memory of our good friend Matthew who passed away ten years ago.
The cycle covered roughly 600km, went through four countries (England, France, Belgium and Netherlands) and took place over four days. It was a challenge we all wanted to do well on, having only two punctures the whole trip was unbelievable, and, thanks to the Belgian and Dutch cycle pathway system, we remained safe and crash free throughout. I say crash free, one of the group did manage to go over the handlebars cycling off the ferry, right in front of the 300 cars waiting to get off too…I didn’t stop laughing until Amsterdam (Matthew would’ve done the same). We saw some beautiful sights from windmills in Netherlands, canals in Belgium and beaches in France. We even managed to cycle some of this year’s Tour de France route.
Our event received over 360 individual donations, and the total raised is inching towards £13,000, all going towards Young Lives vs Cancer. But why did we choose them as our charity?
Young Lives vs Cancer is a charity which was exceptionally supportive to Matthew and his family through his diagnosis, treatment and ultimately in his passing. They provided information, advice, and bereavement support, they can offer free stays for family when treatment is away from home and financial advice for anyone who needs it. COVID-19 has hit all charities exceptionally hard, and this one in particular has a special place in our hearts, it’s the least we could do for them.
Whilst we are over the moon to be able to generate money for the charity, what was most special to me was being able to spend time together as a group. We don’t often all get together for a long stretch of time and being able to talk about the good (and bad) times, reminisce about Matthew and ultimately continue to keep his memory alive is what makes these trips, and challenges even more special. Even after ten years, time together with friends and family helps with the grieving process.
Thank you, Aurora, for allowing me the time to complete this trip, and thank you to everyone for the donations.
The holy grail of agency acquisition
Under what circumstances would Neil and I sell our pride and joy, Aurora Healthcare Communications? We have sometimes debated this after 17 years of running the business, and in theory, it required five key factors to be in place: The ability to still grow our business to provide the breadth of expertise our clients need More…
Under what circumstances would Neil and I sell our pride and joy, Aurora Healthcare Communications? We have sometimes debated this after 17 years of running the business, and in theory, it required five key factors to be in place:
- The ability to still grow our business to provide the breadth of expertise our clients need in a fast-changing healthcare landscape
- The opportunity to add new services and specialties to meet these client needs
- Ensuring our staff have a great experience, greater opportunities and the same great culture
- The prospect of still being involved in the strategic direction of the business
- Ideally, partner with friends who we like and trust.
The first four are promised by everybody that approaches you to acquire your business; the fifth is what makes those a certainty. And this is why we said ‘Yes’ to our long-time friend and colleague, Jonathan Wilson, owner of Spectrum in the US, when he asked us to join him in his quest to provide first-class service and capabilities to healthcare clients globally.
Together we can now provide the full range of agency services to clients on both sides of the Atlantic, and through our 15-year-long working relationship as Global Health Marketing & Communications (GHMC) partners, we know we work well together and can call on our other partners worldwide to provide knowledge on the ground in 60 key markets.
We will be growing, adding new capabilities, and bringing in new expertise to the London office. We will be expanding how we can support our clients. Neil and I will remain in the business with the same leadership led by MD Chris Bath, and the whole team will see positive changes and new opportunities with a continuing focus on the award-winning impact culture we have created. And we will be doing all this in partnership with friends with whom there is mutual trust and respect and who have a proven track record of building a unique and brilliant full-service consultancy. We can’t wait to build the same in the UK, continuing to shape healthcare communications practices into the future.
Today Spectrum and Aurora come together as GHMC Companies, each still offering the independent consultancy experience our clients know and love, with founders in the business and quality top of mind. It doesn’t get better than that, does it?
Keep watching to see how we continue to help our clients improve more lives and prove it. Or better yet, experience Aurora for yourself.
Back Together Again at a Real-World Congress

Learnings from Aurora at ERA, Paris We recently had the pleasure of attending the ERA 2022 Congress on behalf of our client, the Eur Association, to run the media and KOL engagement, press briefng, and ensure the running of an press offce. ERA this year was a hybrid Congress, meaning we were working hard to More…
Learnings from Aurora at ERA, Paris
We recently had the pleasure of attending the ERA 2022 Congress on behalf of our client, the Eur Association, to run the media and KOL engagement, press briefng, and ensure the running of an press offce.
ERA this year was a hybrid Congress, meaning we were working hard to ensure the Congress content were accessible in tailored formats for both virtual and real-world journalist and KOL attendees
Two members from our team attended onsite in Paris whilst wider team members supported from Auro business has begun to get back to in-person events and start to resemble normality once again. virtual attendees. The experience was a truly inspiring one as this marked one of the frst re
So, congresses are back! But what can we learn from our experiences being back on site:
Back together, accelerating science
The message of ‘togetherness’ is a strong one and it’s coming through loud and clear fr academic communities, and the media. Unsurprisingly, everyone was happy to be back on-site, netw information, and engaging in thought-provoking scientifc discussions in a far more human way. bringing communities back together again in the common interest of furthering and accelerating s Having gone through a global pandemic together, the principles of collaboration, co-creation, an stronger and more relevant than ever.
Immersive tech is commonplace
On many Pharma exhibition booths was a show-stopping piece of technology, designed to enhance un treatment and disease area with deeper, immersive learning. The most prolifc vehicles that we Augmented Reality and Virtual Reality.
Hybrid must be here to stay
the importance of accessibility to information, highlighted at ERA, means the ‘behind a close yester-year is offcially dead. Some of the oral poster sessions and key presentations were be researchers own labs and homes to a mix of real-world audiences and virtual attendees. Some sess blend of speakers on stage joined by a panel of real-world and virtual speakers and presenters.
Doing our bit for the planet
Through rooting principles such as being a paperless Congress at the heart of the event and ensu through carbon offsetting, we can make sure we are all doing our bit to maximise real-world netw with the sustainability and environmentally-friendly benefts of virtual work. But we’ve got one nagging question remaining, will medical congresses soon include Metaverse kooky but it’s already happening elsewhere!
Avatars at the ready!
Aurora collaborates to win another patient support award, helping the one million people who live with heart failure
Last week’s highly regarded Pharmaceutical Market Excellence Awards (PMEAs) featured incredible examples of the impact we can make to the lives of patients, families and healthcare professionals. Congratulations to all the winners and nominees. We are thrilled to have been there and to have brought home the award for Excellence in Patient Education and Support collaborating with More…
Last week’s highly regarded Pharmaceutical Market Excellence Awards (PMEAs) featured incredible examples of the impact we can make to the lives of patients, families and healthcare professionals. Congratulations to all the winners and nominees.
We are thrilled to have been there and to have brought home the award for Excellence in Patient Education and Support collaborating with Novartis, The Clarion Portfolio and Salt.
Fighting Failure: Reprioritising Heart Failure Care in the UK
Heart failure (HF) is a condition that is becoming increasingly prevalent but is poorly recognised. Almost 1 million people in the UK are currently living with HF, with a further 200,000 new patients diagnosed each year.
With a disparity of care across the country, we had to act and create a campaign that would increase the level of understanding of HF in the UK and drive improved diagnosis, care and quality of life for patients. In-depth research and insights gathering confirmed that there was a significant challenge ahead of us. We needed to create a campaign to drive change in HF, but we knew we could not do this alone.
Collaborating closely with healthcare professionals and patients was key and the only path that could make a difference. With partnership at the heart of the campaign, the strategic direction became clear. By the people, for the people.
The Fighting Failure campaign has created practical resources for the HF community and a spirit to help motivate those living with the disease to seek improvement in their quality of life.
As the judges’ commented: “It had bold ambition across UK stakeholders and focused on the need for information. Exceeded expectations.”
If you would like to find out more about our award-winning work to support patients, please get in touch.
A step in the right direction: Aurora’s commitment to sustainability
We’re proud to announce that we’ve achieved the Planet Mark Year 1 Business Certification. This is an incredible achievement involving the entire business. The Planet Mark Business Certification is an internationally recognised sustainability certification for business acknowledging continuous progress, encouraging action and building an empowered community of like-minded individuals. In this crucial #DecadeofAction, measuring our More…
We’re proud to announce that we’ve achieved the Planet Mark Year 1 Business Certification. This is an incredible achievement involving the entire business.
The Planet Mark Business Certification is an internationally recognised sustainability certification for business acknowledging continuous progress, encouraging action and building an empowered community of like-minded individuals.
In this crucial #DecadeofAction, measuring our own carbon footprint has been a critical step in reducing our impact on the planet and society. Yesterday the whole team participated in an interactive sustainability workshop to kick off our planned activities.
Through Planet Mark we have protected an area of endangered rainforest thanks to Cool Earth; a charity working alongside rainforest communities to halt deforestation. Our pledge through Cool Earth goes directly towards supporting the Asháninka community in Central Peru.
Through our commitment to Planet Mark we are also helping the Eden Project – an educational charity building connections with each other and the living world, exploring how we can work together towards a better future.
We want to continue to have a positive impact through our business and hope that we can empower our community to take climate action. Each and every one of our team has contributed to our achievement in becoming Planet Mark certified, and will continue to play an important role in our sustainability commitment.
Claire comments:
“We are a small business but nevertheless dedicated to doing what we can to protect people’s futures. We are a healthcare specialist communications agency and improving lives through better health information is what we do every day. This goes hand in hand with sustainable living and protecting our planet, for ourselves and for our clients. In fact, This is Avalon Group companies all work together with their clients to achieve Healthcare for Good via an ethical framework to ensure eco-friendly practices as well as diversity of thought and creativity. Nothing we recommend should be harmful to people or the planet, so it requires objectivity and integrity to ensure we are always doing the right thing to improve people’s health. We are proud to achieve PlanetMark certification and look forward to reducing our carbon footprint year-on-year.”
We encourage you to get in touch if you have any questions or suggestions you’d like to share with us, or to join us on this exciting journey of sustainability. Together, we are a collective force for good.
Creating bespoke communications: Identifying the “something”

Earlier this year, Arvinas and Pfizer announced their new collaboration to develop and commercialise a proteolysis-targeting chimera (PROTAC) molecule.[i] Arvinas was the first company to ever get a PROTAC to a human clinical trial in March 2019, and this is the second PROTAC it has brought to clinics. PROTACs initiate protein degradation by kicking the body’s More…
Earlier this year, Arvinas and Pfizer announced their new collaboration to develop and commercialise a proteolysis-targeting chimera (PROTAC) molecule.[i] Arvinas was the first company to ever get a PROTAC to a human clinical trial in March 2019, and this is the second PROTAC it has brought to clinics.
PROTACs initiate protein degradation by kicking the body’s cellular waste disposal system into action to dispose of harmful proteins. The potential therapeutic applications for PROTACs are numerous, and there are 15 PROTACs in various stages of clinical trials. Whilst all but one of these trials are in cancer, researchers are investigating the use of PROTACs in Alzheimer’s, dementia, heart conditions, diabetes, bacterial infections and much more.
However, as with any advanced therapy, they are more challenging to talk about than conventional therapies throughout the healthcare system, from pricing to prescription, which makes them difficult to reach patients.
We are constantly bombarded with adverts, emails, WhatsApp messages, notifications, social media posts. Audio-visual overload means it is crucial that we only communicate the essentials to our audiences. What is it? And more importantly, why should they care? As we move into a more complex healthcare environment, we must remember that everyone doesn’t need to know everything. Something needs to stand out for them to care, and that something needs to be communicated in a way that is easily understood.
What does this mean for communications?
As therapies become increasingly complex, we may be able to help ever-more specific patient populations. When communicating complex topics, the audience must be laser-focused at the front of our minds. What do they need to know? The levels of information required by patients will be vastly different to the public, and a “one-size fits all” approach often results in low engagement. Communicating to other audiences, such as healthcare professionals, often requires substantial nuance. They may not need to understand the intricacies of every new therapy, just what is relevant to their patients and practice.
If you ask a patient what they would like to know about a PROTAC treatment they were being offered as part of a clinical trial, they may want to understand how this treatment differs from others available and what makes it better? We would have to find a way to explain PROTAC’s unique mode of action, destroying harmful proteins, opposed to inhibiting the production of proteins. Of course, they may want to know something completely different, which is why it’s important to ask our audience what they want to know. That way, we can create truly bespoke communications solutions.
George Tannenbaum touches on this in an instalment of his Ad Aged blog, where he says it’s our job to turn every page,[ii] intimately understand our client’s brand and market, and then pick out that something that differentiates it from the rest of the crowd.
At Aurora, we use an insight-driven approach to communications. We have a wealth of experience distilling complex information about patient experience, treatments, markets, and disease landscapes to insights that can ultimately improve lives.
If you want to find out more about how we reach and activate audiences, then get in touch: joshua.vine-lott@auroracomms.com
References
[i] Press release: Arvinas And Pfizer Announce Global Collaboration To Develop And Commercialize Protac® Protein Degrader Arv-471. July 2021. Available at: https://www.pfizer.com/news/press-release/press-release-detail/arvinas-and-pfizer-announce-global-collaboration-develop
[ii] George Tannenbaum. Ad Aged. Read every page. https://adaged.blogspot.com/2021/09/turn-every-page.html?utm_source=feedburner&utm_medium=email&utm_campaign=Feed%3A+AdAged+%28Ad+Aged%29
What does building a culture of innovation mean anyway?
While we were away as a company last week, enjoying being together again and investing in our culture, we were recognised for the importance we place on our people by an esteemed group of judges from the Business Culture Awards. We beat off some tough competition to win the Building a Culture of Innovation Initiative. It was More…
While we were away as a company last week, enjoying being together again and investing in our culture, we were recognised for the importance we place on our people by an esteemed group of judges from the Business Culture Awards. We beat off some tough competition to win the Building a Culture of Innovation Initiative. It was a strong entry, with clear measurable outcomes for our business, but what exactly does it mean?
Culture and Innovation are two overused business buzz words. I want to share what they mean to us.
First culture. This is not something we believe can just be created or improved with wellbeing measures, a values revamp, or cool social activities. Culture comes from the top. In our case, it is aligned to the values that Neil and I have always held dear since we started Aurora 16 years ago. Principles and behaviours that we expect everyone on the team to feel the same way about. Things like not putting yourself before the team, doing what you say you’ll do, thinking bigger for clients, and coming wholeheartedly to work are what shape our culture. People are recognised for these behaviours by colleagues as they live them every day, and part of the culture of innovation we were recognised for was also letting people know when they weren’t being culture aligned. Of course, it is easier for the culture to come from the top when the business is owner led and managed. Far trickier when the ones that ‘set’ the desired culture for the business are not leading it.
Innovation. The best definition I have ever heard is from the great Dave Hall from the Ideas Centre who says that for something to be innovative it must be both novel and useful. Such a clear and simple description. It certainly applies to this award win, where the programme we put in place in March last year has proven to be both. New ways of working have improved business outcomes, even when we were unable to be together in person. We put our people first, and it has paid back in bucket loads, with improved creativity, autonomy and decision making.
Everyone embraced the changes as well as the intention behind them, which contributed to the success. But we still have a way to go. Continuous improvement is also part of our culture, so we are not going to stop here. Culture and innovation will fuel and inspire the next phase of growth for our group of businesses. We couldn’t have got to this point without the help of Corporate Punk working as partners through this journey. It is their Culture Index that set the course and measured its success, and their unfailing desire, like ours, to get it right for the people that won this prize.
If you’d like to talk to us about creating a company culture of innovation or want to experience our culture first-hand then get in touch.
Inthemiddleism, is that even a word? No, but let me explain a bit about what it means to us
Here it is – Aurora’s refreshed brand. We’ve been working on this since February, and we’re thrilled to finally share it with everyone. But in truth, this is more than a refresh. It’s more of a reminder. As one of the longest running indy healthcare communications agencies, Aurora has become known for great work. But we More…
Here it is – Aurora’s refreshed brand. We’ve been working on this since February, and we’re thrilled to finally share it with everyone. But in truth, this is more than a refresh. It’s more of a reminder.
As one of the longest running indy healthcare communications agencies, Aurora has become known for great work. But we wanted to be known for being one of the best, and to do that we made ourselves a promise – to be ‘bold, brave and brilliant’. In everything. From bringing in the best talent, to only partnering with clients who want to make a difference.
That’s our identity, it’s in our DNA. And now, it’s in our brand. It’s in our nature to do work that makes a real difference, work that helps clients to innovate, work that doesn’t sit “in the middle”.
We deal with matters that profoundly affect people’s lives, so we can’t be shy when we design communications programmes that reach, inspire and activate communities, patients, families, doctors, nurses. Anyone affected by anything in health. We want to improve lives and prove it through communications, and to do that we can’t break our promise to be ‘bold, brave and brilliant’.
What does that promise mean for clients and for people who want to join us?
Well, if you’ve ever thought about giving us a call, now’s the time to do it. We’ve got a fantastic team from account coordinator right the way up to our leadership group. If you want to improve lives and prove it, let’s get to work.
PS, I couldn’t close this without saying thank you to those that have made this rebrand happen. Neil Simpson, Finer Vision, Julia Burns, Helen Hay and Sam Bevans – incredibly talented individuals who came together to make this possible.
Aurora bolsters leadership team with new appointment
Strategic communications consultancy Aurora announces a senior hire to add to its leadership team. Sebastian Stokes joins as Director to concentrate on accelerating growth across Aurora’s three practices, focusing on diversification and digital. The appointment comes at an important time for Aurora, as the agency sets its eyes on further expanding services and expertise to More…
Strategic communications consultancy Aurora announces a senior hire to add to its leadership team. Sebastian Stokes joins as Director to concentrate on accelerating growth across Aurora’s three practices, focusing on diversification and digital. The appointment comes at an important time for Aurora, as the agency sets its eyes on further expanding services and expertise to clients.
Seb has run SHED Communications for five years, a communications consultancy which specialises in consumer health and patient engagement both in the UK and globally. A key area of focus is digital and social media innovation, with clients including the World Health Organization, Pfizer, the British Coffee Association and several FMCG brands.
Seb says: “I’m incredibly excited to be joining the Aurora team, particularly as their ambition really stands out in the industry. The health space has evolved rapidly in the past year for obvious reasons and Aurora is exceptionally well positioned to deliver insightful, data-driven and creative communications – exactly where I want to add value for client organisations.”
Aurora advances
Aurora has seen a busy year to date, including the promotion of Chris Bath to Managing Director, a growing team and significant new business wins. A larger Farringdon office to aid collaboration is also on the way. Chris says: “We’ve had a positive start to 2021, including client wins ranging from med tech and devices to some of the most exciting pharma innovations, and importantly we have a vision to be bold, brave and brilliant in everything that we do over the next few years. It’s the ideal time to add Seb’s strategic and digital skills to the senior team.”
Claire wins Healthcare Communications Leader at Communiqué 2021
We are very proud to announce that Aurora’s CEO Claire Eldridge has been named Communiqué 2021 Healthcare Communications Leader. We know first-hand what an outstanding leader she is. Not only has Claire supported everyone at Aurora and the other healthcare businesses in the This is Avalon Group throughout the pandemic, but she’s continued to create a successful, growing More…
We are very proud to announce that Aurora’s CEO Claire Eldridge has been named Communiqué 2021 Healthcare Communications Leader.
We know first-hand what an outstanding leader she is. Not only has Claire supported everyone at Aurora and the other healthcare businesses in the This is Avalon Group throughout the pandemic, but she’s continued to create a successful, growing group of companies during challenging times.
This is how the Judges on the night described her:
“Claire is a true leader, who has shown huge breadth in terms of her professional and personal achievements. After successfully running Aurora for 15 years, Claire has undertaken a restructure of the organisation that was aligned to client needs, truly differentiating the company. Her approach is not only authentic but also passionate – her dedication to her team and business is truly remarkable, making her more than worthy of winning this award.”
And we couldn’t agree more!
The celebrations continue
It was a great night for Aurora at Communiqué 2021, the industry’s first post-pandemic, real life, COVID-friendly awards ceremony, as we were also finalists in:
- The Excellence in Healthcare Partnerships category for our work with Bristol Myers Squibb. Our team developed a Back-to-Work Guide in partnership with people who have directly experienced, and overcome, the challenges of head and neck cancer. This cancer and its treatment can have life-changing consequences for patients’ appearance and ability to communicate, as well as mental health.
- Excellence in Patient Programmes for our work with Novartis. The Fighting Failure: Reprioritising Heart Failure Care in the UK campaign created practical resources for the heart failure (HF) community and a spirit to help motivate those dealing with the disease’s challenges to seek improvement.
To hear more about either of these programmes of work or more about us and all the work we do, please do get in touch.
Tackling racial health inequalities – what can we do?

What does it mean to be unequal? Inequality is the state of not being equal, especially in status, rights, and opportunities[i]. Inequalities exist throughout our society and are often systemic, leading to unfair and unequal opportunities. Defining moments in time can help to highlight certain inequalities, increasing awareness of the problem, and rallying people around More…
What does it mean to be unequal?
Inequality is the state of not being equal, especially in status, rights, and opportunities[i]. Inequalities exist throughout our society and are often systemic, leading to unfair and unequal opportunities. Defining moments in time can help to highlight certain inequalities, increasing awareness of the problem, and rallying people around a just cause. We have seen this recently with the conviction of Derek Chauvin for the murder of African American, George Floyd. This may be a small step in hopefully supporting a move away from racial inequalities, but there is still a lot of work to be done. The same can be said for health inequalities. We recently watched Tortoise’s ThinkIn ‘Can Covid cure healthcare of its race bias?’ in which speaker Dr. Mohammad Razai, Academic Clinical Fellow in Primary Care at St George’s University of London, said, “We have known about ethnic inequalities in health, sometimes known as health disparities for a very long time.” It’s important to note at this point that health inequalities stretch far beyond race, and discrimination affects all parts of our society, from gender to sexual orientation. However, in this blog, we will focus on the role we play in addressing racial health inequalities. Whilst COVID-19 has brought racial health disparities to the forefront of conversation, for example, data published in January this year revealed that black African males are 2.7 times more likely to die from COVID-19 than white males,[ii] these inequalities are not something new. We know that ethnic minorities have poorer access to healthcare and poor experiences of care and treatment[iii] related to racial discrimination and marginalisation.[iv] This contributes to mistrust between ethnic minorities and the NHS, making them less likely to seek medical help / advice. Ultimately, this results in poorer health outcomes. For example, black women are four times more likely to die during pregnancy or childbirth than white women.[v]
What can we do?
It can be difficult to look at such a complex problem and understand what we can do to evoke positive change. That said, we believe that our role as communicators is to build and establish trust with ethnic minority communities. For example, it’s often easier to recruit patients that are highly engaged with their health for co-creation projects. These patients are usually white, British and from higher socioeconomic backgrounds, which can result in under representation of minority ethnic groups in the end product. By aiming to include patients from diverse backgrounds in our communications programmes, we can build a more holistic picture of the patient experience. This will ultimately help us to create materials, messaging and campaigns that benefit a larger proportion of the patient population. Reaching out and interacting with minority communities also builds trust, as their experiences are not only heard, but acted upon to improve outcomes. We must act to drive change in our industry, first and foremost by educating ourselves about the inequalities that exist (see further reading at end of this post), and then by acting to address them. Tackling health inequalities is understandably no simple task. There is not a simple answer, and it is hard to look at healthcare in isolation when systemic racism exists across society. The impact is felt in employment, education, and criminal justice. But we need to start somewhere, and COVID-19 has put the spotlight on healthcare, providing impetus to bring about long-awaited change.
Knowledge is power
If you want to know more about health inequalities, the reasons behind them, and what can be done to address them, here are some great resources:
- Tortoise ThinkIn – Can Covid cure healthcare of its race bias?
- Health Equity in England: The Marmot Review 10 Years On
- Build back fairer: The COVID-19 Marmot Review
- Sway – Unravelling unconscious bias. Dr Pragya Agarwal
Please get in touch if you would like to learn more about how we at Aurora ensure that minority communities are not only reached, but actively engaged in our campaigns. We’d love to hear from you.
References
[i] Alkire, S., Foster, J., Seth, S., Santos, M. E., Roche, J. M., and Ballon, P. (2015). ‘Multidimensional Poverty Measurement and Analysis’, Oxford: Oxford University Press. Retrieved on 2 October 2015 from Oxford Scholarship Online: August 2015 [ii] Office for National Statistics. Updating ethnic contrasts in deaths involving the coronavirus (COVID-19), England and Wales: deaths occurring 2 March to 28 July 2020. October 2020. Available at: https://www.ons.gov.uk/peoplepopulationandcommunity/birthsdeathsandmarriages/deaths/articles/updatingethniccontrastsindeathsinvolvingthecoronaviruscovid19englandandwales/deathsoccurring2marchto28july2020 Last accessed: May 2021 [iii] Stead M, Angus K, Langley T, et al. Mass media to communicate public health messages in six health topic areas: a systematic review and other reviews of the evidence. NIHR Journals Library, 2019. Public Health Research No 7.8. Available at: https://www.ncbi.nlm.nih.gov/books/NBK540706/[iv] Paradies Y, Ben J, Denson N, et al. Racism as a determinant of health: a systematic review and meta-analysis. PLoS One2015;10:e0138511. doi:10.1371/journal.pone.0138511 pmid:26398658 [v] MBRRACE-UK. Saving lives, improving mothers’ care. December 2020. https://www.npeu.ox.ac.uk/assets/downloads/mbrrace-uk/reports/maternal-report-2020/MBRRACE-UK_Maternal_Report_Dec_2020_v10.pdf.
Aurora names Chris Bath as new managing director to spearhead agency’s evolution
Below is very exciting news to start our year. Please see the communication which has been distributed today. LONDON, 11 January 2021. Chris Bath has been promoted to managing director at strategic communications consultancy, Aurora, to lead the team as it adapts to today’s healthcare communications challenges. Chris says: “As an independent agency, we evolve More…
Below is very exciting news to start our year. Please see the communication which has been distributed today.
LONDON, 11 January 2021. Chris Bath has been promoted to managing director at strategic communications consultancy, Aurora, to lead the team as it adapts to today’s healthcare communications challenges.
Chris says: “As an independent agency, we evolve fast in times of change and so enable our clients to innovate and pivot quickly too. That ability has never been more important than now.”
Claire Eldridge, CEO, comments, “Chris is the ideal person to lead this charge, both from a cultural and capability perspective. He provides excellent counsel, champions evaluation, and lives our company values every day. In doing so, he enables our healthcare clients to communicate effectively and so achieve better patient outcomes – which is what Aurora is all about.”
Chris joined Aurora in 2015 and achieved rapid promotion to the agency’s Management Team. As well as providing senior counsel to clients and agency teams, he led the development of the agency’s digital insights capability and recently launched its measurement practice, Acumen, which helps clients prove the impact of their communications.
Chris adds: “The pandemic has fundamentally changed how patients need to be engaged with, but I also believe it has altered what they want communicating to them, as people become more interested than ever in the science behind treatments. I’m excited to spearhead the way forward for our clients, as they make bold, brave decisions to adapt their communications and engagement with patients and healthcare professionals.”
About Aurora
Aurora was founded in 2005 by Claire Eldridge and Neil Crump. Fifteen years on, it remains fiercely independent. An example of this in action is the recent launch of sister consultancy Atlas, which supports clients to connect with patients and advance products and services through strategy, co-design and organisational change services.
Aurora has helped over 100 ambitious organisations solve complex problems, navigate the world’s fast-changing health landscape, and reach and build trust with the audiences that matter. Despite the pandemic, it has continued to hire and promote to build its team of 28 communications experts.
Aurora is the sole UK agency and European hub for GLOBALHealthPR, the largest independent health and science communications agency partnership worldwide.
Find out more…
www.auroracomms.com
www.linkedin.com/company/aurora-healthcare-communications
Notes to editors
Please get in touch with any questions, to set up an interview or for visuals to accompany this release.
Sarah Nixon, Director of Operations, sarah.nixon@auroracomms.com, +44 (0) 7809 127 499
hello@auroracomms.com
We are 15!
Social media was in its infancy. YouTube had only just been launched. Dr Who relaunched. James Blunt was the biggest musician of the year. Needless to say, 2005 was a long time ago but it was when Aurora first launched and we’re still going strong! To celebrate, we recorded this video with our team today More…
Social media was in its infancy. YouTube had only just been launched. Dr Who relaunched. James Blunt was the biggest musician of the year. Needless to say, 2005 was a long time ago but it was when Aurora first launched and we’re still going strong! To celebrate, we recorded this video with our team today talking about what Aurora means to them:
As you no doubt know, Claire Eldridge and Neil Crump, launched Aurora after having worked together and seeing a gap in the market for a strategic healthcare communications agency that was bold and creative. Since then, we’ve helped over 100 companies across the healthcare lifecycle, including most recently helping clients, healthcare professionals and patients adapt to COVID-19. As Claire says, “Pharma and healthcare have never been so vital to the world and we are more driven than ever by our purpose to change patient lives.”
The Aurora Story
It was at the PMEA awards fifteen years ago that we officially launched and, coming full circle, the agency is a finalist for two awards at this week’s ceremony. There have been many other awards, including winning the Communiqué Small Independent Consultancy of the Year and Communications Consultancy of the Year in successive years.
We have always strived to be at the forefront of the healthcare communications industry, and are proud to have:
- Turned around NICE decisions
- Added products to guidelines
- Successfully launched many healthcare “firsts”, including the first pill in multiple sclerosis and the first genetic modifier in cystic fibrosis
- Led the charge when social media was taking off as the first healthcare communications agency to have a Twitter account and a blog
- Worked to speed up access to innovative medicines and technologies, including contributing to the UK government’s Accelerated Access Review
- Championed greater collaboration across the industry
What’s next?
Neil says, “Over the next 15 years, healthcare and communications are going to change dramatically, they will be almost unrecognisable. But one thing that will undoubtedly continue to be absolutely fundamental is partnering meaningfully with patients.”
Claire adds, “As the only independent healthcare agency with our levels of experience, we are positioned to innovate and adapt quickly in these times of change. We will continue to improve lives and prove it, truly transforming the world of patients and industry professionals.”
Here’s to the next 15 years!
Science makes vaccines possible. We make their use real
Immunisation saves lives. It protects you, your family, and your community. Immunisation helps protect future generations by eradicating diseases. Recent history shows that thanks to major vaccination programmes we have been able to eradicate deadly diseases such as tetanus and diphtheria. However, as we have all become increasingly aware, new infectious diseases are appearing around More…
Immunisation saves lives. It protects you, your family, and your community. Immunisation helps protect future generations by eradicating diseases. Recent history shows that thanks to major vaccination programmes we have been able to eradicate deadly diseases such as tetanus and diphtheria.
However, as we have all become increasingly aware, new infectious diseases are appearing around the world. This World Immunisation Week, the focus is, quite rightly so, on the battle we are fighting against Covid-19 and the importance of being vaccinated against this deadly virus.
The science community must re-gain the public’s trust in vaccinations
There is a lack of trust in vaccines by the public, in part due to myth and misinformation spread in all forms of media. This makes vaccine education more important than ever.
In the UK, we have been one of the lucky few to have a relatively smooth vaccine roll-out programme and we are starting to see the benefits. Unfortunately, this is not the case globally. Despite this, we must all do our part to correct misinformation spread online and use effective campaigns to cut through the online noise.
We feel that Pfizer and BioNTech’s recent campaign – #becauseofthis – does exactly this. It is a clever use of emotion to build vaccine confidence amid misinformation and widespread scepticism. The campaign comprises four films featuring footage of real people’s personal moments found online. These spontaneous moments of togetherness were chosen to remind viewers of the moments we all hope to return to once people are safely vaccinated.
At Aurora, we took inspiration from this, and asked our colleagues who have had one or both doses of the vaccine to share what they are most looking forward to being able to do once they are fully vaccinated:
“I am looking forward to feeling more confident and relaxed in social situations with friends and family. Our local football team Fisher Athletic may have a game in May where a crowd will be allowed so I am looking forward to a returning to some normality. I also find that saying goodbye is really weird now. You just kind of walk away. There is no real closure. Bring back the hug!” Lisa Carroll – Office Manager
“In an ideal world it I am most looking forward to being able to take my kids into London, travelling abroad again and visiting family and friends.” Sarah Pritchard – HR Business Partner
“For me, it’s all about hugging. I miss that and although I’ve had hugs at home, I can’t wait to hug my parents and for them to hug my son” – Claire Eldridge – CEO and Co-Owner
“Things I’m especially looking forward to are seeing live music again and eating out. Also, my sister is expecting a baby in July, so looking forward to being able to visit her when the baby arrives (especially as vaccine now being offered to pregnant women) – we haven’t seen each other face to face for well over a year and I missed her wedding last year because didn’t feel confident travelling to that.” – Katherine Diaz – Cheif Finance Officer
Along-side the optimism and hope that this question created, Sam Bevans – Director up a very important point: “I’m conscious that even having been fortunate to have had a first shot, I might still carry and pass on the virus to someone else, even if I’m more protected from it, so I haven’t felt a wave of relief or thought about what I can do having had the jab.”
Vaccines show their true effectiveness and importance once most of the population is vaccinated. Whilst those of us who have been fortunate enough to receive the vaccines can hope for brighter days, it’s evident that we still pose a risk of contracting the virus and passing it on to someone who is not immune yet.
The vaccination against Covid-19 truly needs to be a global effort and we believe that through campaigns such as #becauseofthis and the ABPI’s #ValuingVaccines, pharma needs to lead the charge in driving home the importance of vaccine uptake. After all, vaccines bring us closer.
To get in touch about how we can support you in in disease awareness campaigns and much more, please drop us an email at: hello@auroracomms.com
Digital Health Literacy – a prerequisite competency for the future of effective healthcare

Over just a few months the Covid-19 pandemic has accelerated change in the way companies in all sectors do business. In the healthcare sector, there is a heavy emphasis on the value of digital health throughout healthcare systems. The NHS Long Term Plan had already set a vision for mainstream use of digital services, but Covid-19 triggered an More…
Over just a few months the Covid-19 pandemic has accelerated change in the way companies in all sectors do business.
In the healthcare sector, there is a heavy emphasis on the value of digital health throughout healthcare systems. The NHS Long Term Plan had already set a vision for mainstream use of digital services, but Covid-19 triggered an immediate rise in the use of online health information and services, according to a report by the Good Things Foundation. In March 2020 alone, online consultations doubled from around 900,000 to over 1.8 million.
How can we ensure online initiatives don’t exclude the very people they are designed to empower?
While pharma and the NHS concentrate on developing digital support programmes, and healthtech entrepreneurs on creating all-singing, all-dancing health-enhancing apps, the prospect of digital exclusion looms large.
In September 2020, NHS England asked NHS leaders to review service use and develop digitally-enabled care pathways to increase inclusion; ensure all patients receive the same level of access and care regardless of their digital preferences; and “ensure it does not affect health inequalities for others, due to barriers such as access, connectivity, confidence or skills.” Lessons learned from the Widening Digital Participation (WDP) programme could not be more timely. Recommendations that should be at the heart of a digitally enabled NHS include co-design with those who have low digital skills and face barriers to health care; improving population digital health literacy and support safe and healthy internet use; and improving people’s understanding of how their health and personal data is used.
According to new research from Digital Unite, commissioned by NHS Digital, 11.9 million people in the UK do not have the essential digital skills needed for day-to-day life.
Increasing numbers of web-based patient support programmes assume a level of digital competency that many with long-term health conditions simply do not have. At Aurora, in agreement with the WDP programme, we believe that pharma should act as advocates of digital health literacy in the patient community. We should aim to provide flexible and ongoing digital skills support targeted to the needs of the learner. That might include hands-on help or tuition on how to use online platforms during online ad-boards and patient co-creation panels to ensure that people who are less digitally savvy can participate and voice their needs and preferences. Patients should be engaged at an early stage, even while phase 3 trials are ongoing, to ensure that support programmes meet the needs of the wider patient community.
Existing schemes have identified common barriers such as confidence and skills when using digital platforms and the availability of information online. We believe that if we can overcome these barriers, we can significantly improve health literacy and, in turn, health outcomes.
Ultimately, producers of online health information and digital health initiatives must be mindful of where they are operating and the people they are seeking to support.
In a world of digital first health, we cannot assume that if we build it, they will come. The healthcare sector as a whole must start by building the foundations of equal access and appropriate skills.
If you want to hear more about how Aurora can help you reach your audience, in the right way, get in touch with the Patient Involvement team: piteam@auroracomms.com
Building a health system that’s affordable, effective and ready for what’s next

Recent times have shown that we are all much more resilient, adaptable and open to experimentation than we imagined, both individually and collectively. Our Digital ThinkIn with Tortoise Media explores the question: what can’t we afford to treat anymore? Featuring discussion with Dame Donna Kinnair, General Secretary and Chief Executive of the Royal College of More…
Recent times have shown that we are all much more resilient, adaptable and open to experimentation than we imagined, both individually and collectively.
Our Digital ThinkIn with Tortoise Media explores the question: what can’t we afford to treat anymore?
Featuring discussion with Dame Donna Kinnair, General Secretary and Chief Executive of the Royal College of Nursing, Sir David Nicholson, former Chief Executive of NHS England and Dr Richard Torbett, Chief Executive of the ABPI.
The debate is insightful, often unexpected, and a timely reminder of pharma’s crucially important role in the world.
Pitch perfect? Five steps to an outstanding agency brief

As a client, if you knew that a better brief would lead to a better pitch, would you invest the time? Of course you would (if you could). It’s a question that the Healthcare Communications Association (HCA) – the independent, UK healthcare members-only organisation – recently explored with stakeholders from procurement, marketing, medical affairs and agencies as More…
As a client, if you knew that a better brief would lead to a better pitch, would you invest the time?
Of course you would (if you could). It’s a question that the Healthcare Communications Association (HCA) – the independent, UK healthcare members-only organisation – recently explored with stakeholders from procurement, marketing, medical affairs and agencies as it set about relaunching its Pitching Code of Conduct.
Aurora has more than a passing interest in the topic and our CEO even helped draft the original code a decade ago. So, based on our own experiences and the recommendations of the code, here are five ways to ensure you create a brief that will lead to a successful communication campaign.
1. Go to the top from the off
A couple of years back, we pulled together a breezy 115-slide deck with contributions from a dozen team members to accommodate a two-week proposal deadline. Then came a follow-up brief, offering three working days and a weekend to prepare. The client was itching to get going. They loved our ideas. And then silence. Weeks of radio silence until an email arrived. The proposal was on hold.
Sound familiar? What had happened here was that senior decision makers were excluded from the original development of the brief and had now said, “No”. The budget had not been discussed with them in the first place, let alone signed off.
2. Grant agencies access
What is the point of any pitch if the creative is based on incorrect assumptions? Ahead of sending out a brief, time needs to be ring-fenced for agencies to privately discuss aspects that are specific to their proposed strategy and programme (the HCA recommends a minimum of three weeks, brief-to-pitch, or early submission).
And there needs to be a commitment to ensure agency access to the most senior decision maker pre-pitch and their attendance at the pitch. Without their buy-in, briefs inevitably fall by the wayside. All too often RFPs are circulated – indeed, pitches are won, only for the agency to be told that key aspects of the programme will not proceed, wasting resources, damaging relationships and putting the proposed strategy at risk with a piecemeal approach.
3. Think about measurement from the start
What’s the change you want to see? Clients need to be crystal clear as only then can agencies put in place SMART objectives, evaluation methodology and criteria, and strategies that clearly relate to objectives. Look for agencies with robust measurement processes, such as Aurora, which has been recognised by the PRCA as anaccredited “measurement champion” for Acumen – our healthcare measurement framework combining tools from the International Association for Measurement and Evaluation of Communication (AMEC) and the government.
4. Identify the genuine need
Which brings me to the HCA Code of Conduct first commandment: to “only pitch when we have a genuine requirement for agency support and internal stakeholder commitment to the programme in terms of funding and feasibility”.
5. Bring in an agency to support
Time can be the enemy. It takes senior access and significant head space to write a tight brief that aligns to a strategy. And yet it’s common practice to prescribe solutions without first fully and accurately identifying the problem.
How can we help?
In recent years, we’ve seen requests for proposals (RFPs) accompanied by shorter and shorter response timelines. Sure, the pressure is on in the healthcare industry to deliver, but the potential for good, if not great work increases considerably where due consideration is given to the brief, and an appropriate amount of time is allocated for an agency to pause, reflect and respond.
That’s where we can help. By coming in early, we can work with your team to bring the perspective and the insights that give focus to a brief as well as the desired outcomes. The result of a better brief is that the right work is delivered faster at a lower cost. Get in touch if you’d like us to help with the strategic thinking!
Collaboration – a way of thinking, working, living

A new Aurora report reveals the way ahead for genuine healthcare partnerships. Collaboration is at the heart of successful patient engagement and effective healthcare provision. But in such a complex, nuanced network, true collaborations are rare. So how can we, as an industry, overcome this? In the third and final chapter of our series of More…
A new Aurora report reveals the way ahead for genuine healthcare partnerships.
Collaboration is at the heart of successful patient engagement and effective healthcare provision. But in such a complex, nuanced network, true collaborations are rare. So how can we, as an industry, overcome this?
In the third and final chapter of our series of reports on the topic, find out:
- The common, positive trends we have seen while immersing ourselves in this topic
- The practical and mindset changes needed to move to a more collaborative future
- What we can all do to improve the health discourse across the country
Does representation in healthcare campaigns matter?

It’s 2019 and everywhere we look we can see a pursuit for increased representation of minority groups. Whether it’s in movies, on catwalks, or in parliament, things are changing and for the better. Gone are the days of those campaigns filled with the typical, photoshopped, stock images that marketeers relied on so heavily for so More…
It’s 2019 and everywhere we look we can see a pursuit for increased representation of minority groups. Whether it’s in movies, on catwalks, or in parliament, things are changing and for the better. Gone are the days of those campaigns filled with the typical, photoshopped, stock images that marketeers relied on so heavily for so long.
But is diversity and representation in healthcare campaigns keeping up with the wider world?
Impact on people living with an eating disorder
One example seen in eating disorders suggests no, which as a mental illness has been misrepresented in the media for many years and resulted in a detrimental effect on thousands of people across the UK.
Last week was Eating Disorders Awareness Week. For 2019, Beat, the UK’s largest eating disorder patient organisation, has been focusing on breaking barriers and highlighting that anyBODY can experience an eating disorder. But why?
Because stereotypes and years of misrepresentation have proven harmful for this patient community.
A Beat-commissioned YouGov poll of adults in the UK found:
- 39% believe eating disorders more commonly affect white people
- Six out of ten believe eating disorders mainly affect young people
- 37% of lesbian, gay and bisexual people say they would not feel confident seeking help about eating disorders compared to 24% of straight people
- Only 52% of people from minority ethnicities would feel confident asking for help about eating disorders compared to 64% of white British people[1]
For people experiencing an eating disorder, it can be difficult to seek treatment if they feel they do not meet the expectations of what a person with an eating disorder ‘should’ look like.
The real-life impact of this is that people are not receiving the care they need from healthcare professionals and support systems, leading to depression, isolation, professional and social life destruction, and in some cases, death.
Impact on people living with cancer
This problem extends wider than just mental illness into many disease areas, including cancer.
In England, a research study into the barriers facing ethnic minorities found that there is a distinct lack of health campaigns designed to meet the needs of ethnically diverse people in England. As a result, those groups are presenting to their doctors at a later stage with their symptoms, when prognosis is poorer.[2]
This is also the case for transgender and gender nonconforming (TGNC) people who are often excluded in relation to sex-specific cancers, as highlighted in a Nature paper. It outlined how gendered and stereotypical messaging around breast and testicular cancer meant that the TGNC population were ultimately not informed of their risk, leading to delayed diagnosis and treatment.[3]
This leads us to ask, for campaigns targeted to improve public health or to engage specific patient communities, can we expect a successful result if we are not inclusive? If our communications and materials are not catering for our wider audience, will we be able to engage with people and educate them to uptake helpful and beneficial behaviours? Or will they be left out and feel disengaged with their health and care?
We know that health is important to everyone, but everyone is different, whether it’s by age, sexuality, ethnicity, gender, status or ability. And one size certainly does not fit all.
Whether it’s in our imagery, videos, language or even the channels we use to share content, we need to be critical as to whether we are doing enough to reach, (and ultimately help) our whole audience.
The benefits of representation in this way are not limited to individuals of minority groups, but also to businesses themselves. Diversity can directly influence your credibility and reputation.
And hey, it’s the right thing to do.
Involving patients in your work with Aurora
At Aurora, we follow a robust approach to involve patients in our work. Our methodology recognises that listening is only the first step. We need to co-create with patients – providing multiple opportunities for them to make their voice heard and share experience if we are to design programmes that are aligned to their needs. By understanding the nuances of our patient audience and treating them as partners, we have built campaigns that have made a real difference to wider patient populations.
If you’d like to hear more about how you can involve patients, and represent them in your work, contact patientinvolvement@auroracomms.com
References
[1] Eating Disorders Awareness Week. Available at: https://www.beateatingdisorders.org.uk/edaw [Accessed February 2019].
[2] Niksic M, et al., Ethnic differences in cancer symptom awareness and barriers to seeking medical help in England, Br J Cancer. 2016; 115(1): 136–144.
[3] Combs R, et al., Considering transgender and gender nonconforming people in health communication campaigns, Nature. 2018; 98.
When it comes to innovation, context is king

Innovation should inspire teams, evolve systems and help us take giant leaps forward in the way we live our lives. Innovation is supposed to be useful, seamlessly integrate into our lives and give us our precious time back. Innovation does all of these things when done well. When done wrong it does the opposite of More…
Innovation should inspire teams, evolve systems and help us take giant leaps forward in the way we live our lives. Innovation is supposed to be useful, seamlessly integrate into our lives and give us our precious time back.
Innovation does all of these things when done well.
When done wrong it does the opposite of all of the above and creates a lack of trust and cynicism that, to be honest, we’ve all experienced first-hand.
Unbound 2018, a ‘celebration of innovation’, taught me a few valuable lessons that we should all think carefully about to avoid being a company that over-promises and under-delivers.
Don’t be blinded by all of the data
Rory Sutherland, of Ogilvy-and-industry-fame, walked onto stage with the task of talking about behavioural economics to sum up the state of advertising, marketing and ‘data-driven’ culture.
What data is great at is providing us with insight. It’s predictive and logical, and gives us an amazing view of what might be going on. As good though as data might be at predicting, if we all follow the same logic we’ll all end up in the same place.
Rory cited a great example about Coca-Cola – the number one soft drink company. To logically beat Coca-Cola, you’d go for a cheaper product in a bigger can. If all companies thought like that, you’d end up with a market full of big, cheap soft drinks. What happens when you buck that trend? Well, you end up with the only true long-term contender to Coca-Cola. Red Bull. A product that is more expensive in a smaller can. Where’s the logic in that?
Context is king
The problem with data is that it comes from the past and too much of it makes you miss the most important insights. The art of data-driven creativity is the collision of insights from people, data and context.
If you ignore context you will believe that all ‘gen Z’ers’ will be more competitive and resourceful than ‘millennials’ and to nurture a millennial, you should put them in a team to collaborate, the opposite of what a Gen Z strives for to succeed. (For what it’s worth, we don’t believe in this type of broad segmentation, everyone is different, and we shouldn’t put anyone in a group just because we’re told we have to). We would, therefore, segment based on when they were born, not who they are.
In truth, there is no such thing as a homogenous community. That is where understanding who you are trying to engage with is so important. Where did they grow up; what job do they have; where did they go to school; what’s their favourite brand etc. All of this context changes our perception of who they are and how we might create a programme that is engaging for all who interact with it…and importantly, is truly innovative.
We find ourselves at an interesting point in the way we access information. We’re all picky, and we all know what we want, but innovation can only be innovation if people engage with it.
Innovation then is not about tech or transformation, but about thinking a little differently about how tools and people come together to make a real difference. Deep down, we all know this is true, but hearing it from brands like Lego, Bupa, Unilever and Channel 4 was a really nice reminder that the needs of people must come first.
At Aurora, we don’t just believe that insight helps fuel campaigns, but can help drive strategies that show we have made a real difference. Pop me an email, it’d be great to speak about how we can do this together.
NEW REPORT: Healthcare collaboration in The Age of Enlightened Self-Interest
The final chapter of our report into improving collaboration in healthcare is out now and ready for you to download here. Over the past year, we have written extensively on the importance of collaboration to ensure we have a health system that is fit for purpose. This third and final chapter of our report discusses what More…
The final chapter of our report into improving collaboration in healthcare is out now and ready for you to download here.
Over the past year, we have written extensively on the importance of collaboration to ensure we have a health system that is fit for purpose. This third and final chapter of our report discusses what we have found to be fundamental to effective collaboration and the potential for industry to achieve effective collaboration in the Age of Enlighted of Self-Interest.
Enlightened self-interest is a philosophy described as ‘doing well by doing good’. Many of the issues in healthcare are not black and white; they are many shades of grey. As a result, things are never likely to be perfect. However, as the old saying goes, we must make sure we do not let ‘perfect be the enemy of good’. By focusing on our shared values and bringing different stakeholders to the table to work together, we can think more broadly and use the principles of Enlightened Self-Interest to drive forward healthcare.
There is enormous potential for industry to work with a broader set of stakeholders to contribute a considerable amount to society, while also providing a net benefit to themselves. As we discuss in this piece, we know there is strong evidence regarding the social determinants of health. So could we be in position for the pharmaceutical industry to help address this? For example, could funding improved housing and school meals for underprivileged families could reduce non-communicable diseases and their burden on the NHS, enabling us to spend more on newer, advanced therapies for unpreventable conditions?
Public and private organisations are often seen as uncomfortable bedfellows. There are good ideas and good people on all sides, and as we enter one of the most unpredictable political eras in history, we must utilise each other strengths, and meet in the middle, to make sure we live the healthiest and happiest lives we can.
In the spirit of collaboration, we sought opinions from different sectors to contribute to this report and spending time with people with diverse expertise reinforced just how vital collaboration is. We thank them for their valuable contributions.
You can read all three chapters of Aurora’s report on collaboration here. This marks the beginning of our work in collaboration, and if you would like to discuss it more. Please do get in touch.
Building alliances: the importance of cross industry collaboration

Recently, we have talked a lot about collaboration and its importance in healthcare, for example in my last blog. This was reinforced last week by the King’s Fund, who held an event called Ideas that change health care, to address some of the big questions in healthcare. There was a wide range of fantastic sessions, covering topics from the More…
Recently, we have talked a lot about collaboration and its importance in healthcare, for example in my last blog. This was reinforced last week by the King’s Fund, who held an event called Ideas that change health care, to address some of the big questions in healthcare.
There was a wide range of fantastic sessions, covering topics from the use of artificial intelligence to genomic medicine. However, the final session of the meeting was one which reinforced not only the importance of collaboration, but the importance of looking outside of our own field to do this.
We believe that by involving key stakeholders in healthcare we have the opportunity to work together to improve outcomes. What we saw at the King’s Fund were examples of how involving stakeholders from outside of healthcare can also have amazing results.
Heather Wright, from Aardman Animations (the makers of Wallace and Gromit, amongst many other things) discussed the significance of storytelling and how allegory is a powerful tool for communicating complex issues. This was demonstrated in their moving work Santa Forgot for Alzheimer’s Research UK, which tells a story about the effects of Alzheimer’s disease. Alongside this, Ed Matthews from the Helen Hamlyn Centre for Design presented on the importance of inclusive design, focusing on ensuring that older people are accounted for when healthcare systems are created. These speakers demonstrated how creative and design industry perspective can add a huge amount of value to our work in healthcare.
Dr Tom Fowler from Genomic England then discussed the importance of including the public in the work of the 100,000 Genomes Project to ensure that data is appropriately used. Both Ed Matthews and Tom Fowler really demonstrated the value of including your end audience – something we have also been striving to do through our patient involvement work.
As was pointed out during the day, recent research from the King’s Fund showed that 66 per cent of adults are willing to pay more of their own taxes to fund the NHS.[1] This is an interesting insight into the public view of health, and maybe now we are in a position to start having some difficult conversations about the future of health and how we fund it. Realistically however, we can only do this if we involve all of society closely in the design and running of our health systems, and explain fully why certain decisions are made. If people are involved, they will be invested, if they are invested, they will be more open to difficult conversations.
These speakers all eloquently demonstrated the tough decisions that are ahead and how collaboration and co-creation, across society, is our best hope for ensuring health for all. Collaboration runs through our approach to work and we are always happy to discuss this, whatever challenges you are facing. So, please do get in touch.
Reference
[1]. King’s Fund. What does the public think about the NHS? September 2017.
Available at: https://www.kingsfund.org.uk/publications/what-does-public-think-about-nhs. Last Accessed 08 October 2017.
Aurora and MSD win PMEA for ‘Making Gender Diversity Matter’
We’re thrilled to announce the latest addition to our awards cabinet. Last week’s highly regarded Pharmaceutical Market Excellence Awards (PMEAs) featured incredible examples of the impact we can make to the lives of patients, families and healthcare professionals. Congratulations to all the winners and nominees. We are thrilled to have been there and to have More…
We’re thrilled to announce the latest addition to our awards cabinet.
Last week’s highly regarded Pharmaceutical Market Excellence Awards (PMEAs) featured incredible examples of the impact we can make to the lives of patients, families and healthcare professionals. Congratulations to all the winners and nominees.
We are thrilled to have been there and to have brought home the award for Excellence in Building Corporate Reputation and Trust for our collaborative work with MSD which posed the difficult, but necessary questions that need addressing in gender diversity.
This award recognises us for showing a commitment to making a difference to society and as the judges commented we tackled “an important issue from a different perspective.” They also noted our measurement focus: “The questions asked about gender diversity were spot on, it had a clear strategy and the SMART outcomes were reached or overachieved.”
The award-winning campaign: Making Gender Diversity Matter
What: In the UK, 13% of the science, technology, engineering and medicine workforce is female. But gender diversity is critical for business and economic success. So, we collaborated with MSD to create a campaign to promote better equality by genuinely changing behaviours, moving from conversation and platitudes to proactivity.
How: We brought together thought-leaders from a variety of industries and facilitated knowledge exchange on the burning questions in gender diversity, not the well-trodden, safe ground. We ran a challenging session to tease out those issues and gain real insights. We then amplified the key findings and ideas with in-depth, strategic social media engagement.
Results:
● 84% of attendees believed they had gained real-world insights they could apply to help drive change.
● 92% felt the event broadened their understanding of current thinking on gender diversity.
● Perhaps most importantly, we have seen organisations issue guidance directly based on our findings.
If you would like to find out more about the project or any of our other work, please get in touch at hello@auroracomms.com
Aurora’s Access All Areas Initiative
At Aurora we believe that everyone in the healthcare system with an important role to play in improving access to innovation. All of us can make a difference if we want to, not just for our clients’ benefit, but for society as a whole. As an independent agency, we decided to put our own time More…
At Aurora we believe that everyone in the healthcare system with an important role to play in improving access to innovation. All of us can make a difference if we want to, not just for our clients’ benefit, but for society as a whole. As an independent agency, we decided to put our own time and money into having a positive impact.
Access All Areas is part of our commitment to creating opportunities for improved patient access to innovative and life-changing medicines.
We recognised that despite positive health economic assessment, patients don’t necessarily get timely access to the innovative medicines and technologies they need.
Not content with this status quo, Aurora set itself the challenge to collaborate with the wider healthcare system to determine why this problem persists and, most importantly, to identify and drive meaningful steps that can be taken to improve outcomes.
Aurora has made a three-year commitment to Access All Areas, initially with a UK focus. Our intention is to provide constructive dialogue, fresh ideas and useful, practical guidance for all parties striving towards the common goal of improving patients’ access to medicines.
We change things when we act, when we take just one purposeful step forward.
Achievements to date – Inaugural meeting

Access All Areas was launched in in January 2015 and the inaugural ‘collaborators meeting’ took place on 12 May 2015 at the Royal College of General Practitioners. The meeting facilitated open and challenging dialogue, best-practice sharing and exchange of perspectives. It was attended by nearly 100 professionals spanning the pharmaceutical industry, patient groups and consultancies.
Access All Areas Paper

From Aurora’s bespoke research, stakeholder engagement and commentary at the inaugural meeting, we published a paper called Creating opportunities for improving patients’ access to medicines.
Download the full paper and executive summary.
The paper examines the UK challenge of medicines access. Based on insight gathered from stakeholders across the healthcare spectrum, we identified seven key dependencies, which we believe can positively impact the uptake and flow of medicines.
- Leadership by example
- Planning for alignment
- Contextual decision-making
- Real world data
- Collaboration and governance
- Patient involvement
- Best practice sharing
The dependencies described in the paper point to new behaviours and practices to be adopted across the healthcare environment, and by all its stakeholders.
The paper was not intended as an academic exercise. Aurora wanted it to drive real change and this is already happening.
Accelerated Access Review
The Accelerated Access Review (AAR) of Innovative Medicines and Medical Technologies was announced in November 2014 by the UK Minister for Life Sciences and published in 2016. Its aim was to speed up access to innovative drugs, devices, diagnostics and digital products for NHS patients. Access All Areas made contributions in 2015 to the AAR process, both directly and through the ABPI.
Aurora patient involvement service
As a direct result of Access All Areas and masses of experience in this area, Aurora has formalised patient involvement into a core service. We are now increasingly helping clients look at the reality of the patient pathway and experience and build that knowledge into their programmes. Find out more on about our Patient Engagement service.
The initiative continues…
There are numerous further outputs and offerings in development, so watch this space or, even better, give us a call and get involved! We are currently specifying the detail of a new service to support best practice sharing. Thank you to everyone who has collaborated with us on this.
It is clear that the conditions of medicines access in today’s landscape are a consequence of models of organisational behaviour that have developed over decades. They are the result of our collective making, and so must be the new models we take forward. We need to cross boundaries, forge deeper relationships based on our common goals, and collectively work hard to share the principles that can lead to better practice.
We welcome future collaborations with stakeholders, across the healthcare spectrum, to collaborate on the dependencies we have identified. You may have a particular interest in addressing one or more of these dependencies, or just want to be involved more broadly in future activities.


